Peer Reviewed
Healthcare associated infections (HAIs) are a global problem, causing hundreds of thousands of deaths each year, life-long disability to some survivors, and requiring billions of dollars of additional care. While the rate of device- and procedure-associated infections have shown improvement within United States acute care facilities, greater consideration should be given to other well-established sources of infection; such as the contaminated hospital environment [1].
The link between the environment and HAIs is best explained by what is known as the ‘prior room occupancy risk’ [2]. Patients admitted to rooms that were previously occupied by patients infected with common multidrug resistant organisms (MDROs) such as Clostridium difficile [3] (C. diff), Methicillin-resistant Staphylococcus aureus (MRSA) [4] and Vancomycin-resistant enterococci (VRE) [5] have been found to be at a 2.5, 1.5 and 2.25 times increased risk for developing the same infection, respectively [6]. Since there is no direct contact between the two patients, this risk of infection is almost exclusively associated with the environment. If not properly disinfected, these MDROs can linger on high touch surfaces for weeks to months, serving as a continued transmission risk for many future patients [7].
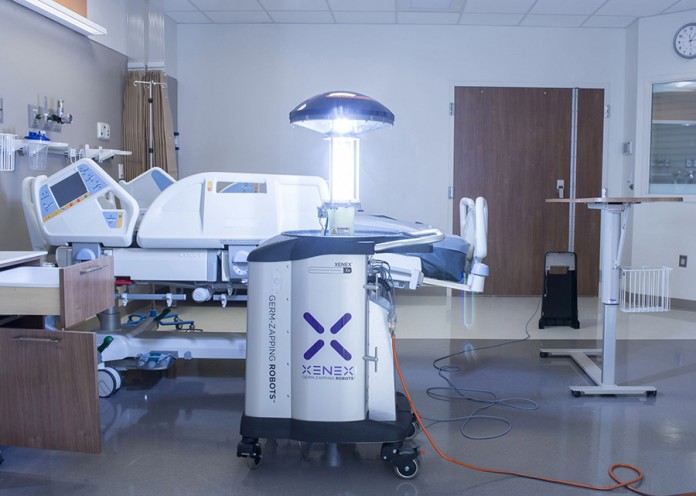
A growing number of healthcare organizations have turned to an innovative pulsed xenon ultraviolet (UV) light technology to complement standard cleaning protocols, with a goal to decrease HAIs. Pulsed xenon UV (PX-UV) disinfection (introduced to the healthcare market in 2010 by Xenex Disinfection Services) is the only UV disinfection technology shown to help hospitals effectively reduce their HAI rates and the body of evidence continues to mount [5-12]. Designed for speed, effectiveness and ease of use, hospital cleaning staff can operate the pulsed xenon Full Spectrum™ UV disinfection robot without disrupting the efficiency of hospital operations. The robot disinfects by releasing pulses of intense UV light spanning the full UV spectrum, destroying viruses, bacteria and bacterial spores in a four-minute disinfection cycle. It has shown to be effective against contagious pathogens, including the Ebola virus and Anthrax spores (as tested in a BSL-4 laboratory at Texas BioMed, San Antonio, TX) [16]. Use of the robot has led to a reported ability to disinfect 30-62 hospital rooms per day; including patient rooms, operating rooms, equipment rooms, emergency rooms, intensive care units and communal areas.
In this article, we will review eight peer-reviewed studies demonstrating the clinical efficacy of the pulsed xenon UV disinfection system to reduce HAIs (Table 1). These outcomes identify important public health implications; estimating the number of infections avoided, as well as associated returns on investment and bed days generated as a result of the infection control interventions involved.
Table 1. Summary of published HAI reduction studies associated with pulsed xenon ultraviolet disinfection systems
| Study Site | Organism of Interest | Healthcare Setting | Incidence Reduction | Estimated Impact |
| Lowell General Hospital [8] | Class I Surgical site infections | Operating Room | 46% | 23 fewer cases in 10,883 procedures |
| Trinity Medical Center [9] | Total Hip/Knee SSIs (Class I) | Operating Room | 100% | 7 fewer cases in 544 procedures |
| Westchester Medical Center [10] | Multiple MDROs | Acute Care | 20% | 185 fewer cases in 22 months |
| Cooley Dickinson Hospital [11] | C. difficile | Acute Care | 53% | 17 fewer cases in 12 months |
| LTAC Facility [12] | C. difficile | LTAC | 57% | 29 fewer cases in 15 months |
| Westchester Medical Center [13] | C. difficile | ICU | 70% | 30 fewer cases in 12 months |
| Cone Healthcare System [14] | MRSA | Healthcare System | 56% | 58 fewer cases in 18 months |
| Orlando Health South Seminole Hospital [15] | Multiple MDROs; C. difficile | Acute Care | 61% | 39 fewer cases in 22 months |
Surgical Site Infections (SSIs) are devastating for patients and pose a significant financial risk for hospitals. Making up over 20 percent of all HAIs, SSIs are the leading type of infection within the U.S. [1]. Alabama-based Trinity Medical Center experienced a 100 percent decrease in class I surgical site infection rates in its orthopedic operating rooms (ORs) after implementing a total joint infection control bundle that included quality improvements and pulsed xenon UV technology to disinfect its ORs and patient rooms [9]. The study states that the intervention may have prevented seven infections, averted one death, and saved $290,990 over the 12 months studied. In a similar fashion, an independent community hospital in the northeastern United States was able to achieve a 46 percent reduction in SSIs following class I (clean) surgical procedures [8]. Thorough terminal disinfection of 13 operating rooms was performed nightly in addition to standard between-case cleaning. The authors estimates the hospital avoided 23 infections and saved $487,055 as a result [8].
C. diff infection is a serious intestinal infection that can cause severe diarrhea, colitis and even death. Many hospital patients, especially those on antibiotics, are susceptible to C. diff. Recent publications funded by the Centers for Disease Control and Prevention (CDC) estimate that C. diff was responsible for over 12 percent of all HAIs within U.S. acute care facilities in 2011 [1]. When applied to all healthcare within the U.S., this organism was responsible for almost half a million infections and approximately 29,000 deaths [3]. Contaminated environments can be a source of C. diff infection, and thus, successful elimination of this associated transmission risk can have an overwhelming public health impact.
One study demonstrated that the use of pulsed xenon UV technology enabled Westchester Medical Center (New York, USA) to reduce hospital acquired C. diff infection rates in its adult intensive care unit (ICU) by 70 percent, potentially avoiding 30 cases over one year [13]. Previously, Westchester published a study reporting that the use of pulsed xenon ultraviolet light technology enabled the facility to reduce HAIs by 20 percent [7]. This decline in incidence occurred even though the hospital disinfected only 24 percent of targeted rooms. The before/after study discovered that the rate of HAIs caused by MDRO and C. difficile was significantly lower during the 22 months of pulsed xenon UV disinfection use compared with the 30-month period prior to implementation of pulsed xenon UV disinfection.
A 2013 study reported that Cooley Dickinson Hospital (an affiliate of Massachusetts General Hospital) experienced a 53 percent decrease in the rate of hospital-acquired C.diff infections after implementing the Xenex room disinfection system [11].
Another study published in 2013 reported on the pulsed xenon robot’s efficacy on MRSA infection rates. The hospital experienced a 56 percent reduction in its hospital acquired MRSA infection rate after implementing an infection prevention program that included the pulsed xenon room disinfection system [14]. Recently, Orlando Health South Seminole Hospital reported a 61 percent reduction in combined VRE, MRSA and C.diff infection rates in its Intensive Care Unit (ICU), an 87 percent reduction in its ICU VRE infection rate, and a 29 percent reduction facility-wide in combined VRE, MRSA and C. diff infection rates after it began using pulsed xenon light technology [15]. The hospital estimates that it saved $730,000 based on the number of C.diff and VRE infections that were avoided [15].
An interesting component of the Orlando Health study is its analysis of the efficacy of pulsed xenon light in two different deployment strategies within the hospital. The difference in infection rate reduction was associated with two different utilization strategies, which provided an indicator for best practices for pulsed xenon disinfection. In the ICU, all discharges and transfers were disinfected with pulsed xenon UV , while non-ICU discharges were disinfected with pulsed xenon UV only under contact precautions for C. diff. As a result, the combined VRE, MRSA and C.diff infection rates decreased 61 percent in the ICU, whereas the non-ICU discharges and transfers resulted in only a 29 percent decrease in VRE, MRSA and C.diff infection rates facility wide.
Environmental contamination may pose a greater challenge in long-term care facilities than acute care settings because of the extended length of stay for patients and patient-to-patient contact. Patients inhabit rooms for weeks to months at a time, making thorough disinfection a challenge for environmental staff. Many hospitalized patients are transferred to and from Long Term Acute Care (LTAC) facilities, increasing the likelihood of acquiring a C. diff infection in the process. The use of pulsed xenon UV in communal living areas and patient rooms at an urban LTAC facility resulted in a 57 percent decrease in C. diff infection, and 29 fewer cases over a 15 month period [12].
Conclusion:
Standard cleaning practices have been shown to be inadequate in removing the dangerous pathogens from the environment that may infect the next patient in that room. Pulsed xenon UV disinfection provides healthcare facilities with a powerful tool to destroy potentially harmful microorganisms – enhancing the safety of patients and healthcare workers. Clinical effectiveness of this technology requires epidemiologically rooted implementation strategies and seamless integration into daily hospital operations, and cannot be overemphasized when considering the validity of UV technology.
Disclosures:
Dr. Mark Stibich is co-founder and Chief Scientific Officer of Xenex Disinfection Services. InfectionControl.tips received no funds and declares no conflict of interest in the publication of this article.
References:
- Magill, S.S., et al., Multistate point-prevalence survey of health care-associated infections. N Engl J Med, 2014. 370(13): p. 1198-208.
- Huang, S.S., R. Datta, and R. Platt, Risk of acquiring antibiotic-resistant bacteria from prior room occupants. Arch Intern Med, 2006. 166(18): p. 1945-51.
- Lessa, F.C., et al., Burden of Clostridium difficile infection in the United States. N Engl J Med, 2015. 372(24): p. 2369-70.
- Mrsa, R., et al., Use of Pulse Xenon Ultraviolet to Deactivate Clostridium Difficile spores , Methicillin. Pulse, 2010: p. 2010-2010.
- Svec, P., et al., Evaluation of (GTG)5-PCR for identification of Enterococcus spp. FEMS Microbiol Lett, 2005. 247(1): p. 59-63.
- Chemaly, R.F., et al., The role of the healthcare environment in the spread of multidrug-resistant organisms: update on current best practices for containment. Ther Adv Infect Dis, 2014.
- Otter, J.A., et al., Evidence that contaminated surfaces contribute to the transmission of hospital pathogens and an overview of strategies to address contaminated surfaces in hospital settings. Am J Infect Control, 2013. 41(5 Suppl): p. S6-11.
- Catalanotti, A., et al., Influence of pulsed-xenon ultraviolet light-based environmental disinfection on surgical site infections. Am J Infect Control, 2016: Epub ahead of print.
- Fornwalt, L., D. Ennis, and M. Stibich, Influence of a total joint infection control bundle on surgical site infection rates. Am J Infect Control, 2016. 44(2): p. 239-41.
- Haas, J.P., et al., Implementation and impact of ultraviolet environmental disinfection in an acute care setting. Am J Infect Control, 2014. 42(6): p. 586-90.
- Levin, J., et al., The effect of portable pulsed xenon ultraviolet light after terminal cleaning on hospital-associated Clostridium difficile infection in a community hospital. Am J Infect Control, 2013. 41(8): p. 746-8.
- Miller, R., et al., Utilization and impact of a pulsed-xenon ultraviolet room disinfection system and multidisciplinary care team on Clostridium difficile in a long-term acute care facility. Am J Infect Control, 2015. 43(12): p. 1350-3.
- Nagaraja, A., et al., Clostridium difficile infections before and during use of ultraviolet disinfection. Am J Infect Control, 2015. 43(9): p. 940-945.
- Simmons, S., et al., Impact of a multi-hospital intervention utilising screening, hand hygiene education and pulsed xenon ultraviolet (PX-UV) on the rate of hospital associated meticillin resistant Staphylococcus aureus infection. Journal of Infection Prevention, 2013.
- Vianna, P.G., et al., Impact of pulsed xenon ultraviolet light on hospital-acquired infection rates in a community hospital. Am J Infect Control, 2015.
- Stibich, M. and J. Stachowiak, The microbiological impact of pulsed xenon ultraviolet disinfection on resistant bacteria, bacterial spore and fungi and viruses. South Afr J Infect Dis, 2016;31(1):12-15












[…] Stibich, M. (2016, May 13). Reduction of HAIs through the use of Pulsed Xenon UV Disinfection. Retrieved July 21, 2016, from https://infectioncontrol.tips/2016/05/13/reduction-hai-pulsed-xenon/ […]