Abstract
Pharmaceutical companies spend an enormous amount of time and resources making sure that their products are safe for the patient. If a sterile drug company fails to do what is expected by a country’s regulatory agency, they will no longer be able to sell product in that country. One of the key best practices in the pharmaceutical industry is validation of all processes to confirm that their procedures to prevent contamination are acceptable before they can manufacture product for sale. A facility is not compliant if they have not confirmed that all processes are repeatable and meet specifications. They also must have established procedures to routinely test finished product, raw materials, water, as well as the environment for contamination. The pharmaceutical industry must take the initiative to prevent contamination of their products and are required to consistently know the ‘health’ of their manufacturing environments so that they do not harm patients.
In the area of environmental infection control, our experts in healthcare have excellent knowledge of which microbes cause infections and also know a lot about reducing microbial contamination with proper cleaning and disinfection. However, most healthcare facilities around the world use infection as the primary indicator of a contamination problem versus performing routine monitoring for high levels of microorganisms in the environment or water before a patient gets infected. Should healthcare facilities be more proactive in their approach to preventing hospital acquired infections and adopt some of the pharmaceutical industries best practices?
Pharmaceutical Industry has Strict Regulations around the World
Clean rooms, restricted access barriers and isolators are all utilized for traditional pharmaceutical manufacturing. These environments are designed to prevent contamination of a drug product. Each cleaning, disinfection, decontamination and sterilization process is validated and routinely monitored by the users to show contamination control. Suppliers offer documentation and support to assist manufacturers but it is the sole responsibility of the drug company to design, develop, validate and monitor their processes if they want to receive regulatory approval to sell product as well as to continue selling product.
Culture methods continue to be the gold standard in the pharmaceutical industry
The World Health Organization (WHO), as well as other individual country regulatory agencies, have detailed guidance on environmental monitoring of clean rooms. Culture methods continue to be the gold standard in the pharmaceutical industry in spite of the slow time to result and questionable sensitivity. WHO’s “Environmental Monitoring of Clean rooms in Vaccine Manufacturing Facilities” describes all of the methods for monitoring microbial contamination as well as frequency and recommended limits of colony forming units (CFU) depending on the classification of the clean room. While a non-sterile drug facility’s environmental monitoring program will not be as stringent as a sterile injectable vaccine, it is still expected to perform monitoring based upon a risk assessment. Even new real time technologies to measure contamination levels require validation against traditional culture methods in order to receive regulatory acceptance.
Lack of Regulation in Drug Compounding = Wide Spread Contamination & Tragedy
The compounding pharmacy market continues to grow due to drug shortages, growing elderly population as well as pain therapy and personalized medicine. Until recently, there was not much awareness of the risk of contamination in compounded sterile drugs. However, the New England Compounding Center (NECC) disaster in the United States is a perfect example of what happens when a sterile drug manufacturer does little to prevent gross contamination of a product. As of 2015, 64 people have died and more than 800 people have been infected with fungal infections.1 The $200 million dollar compensation fund that was granted by the court last year will never be enough even if NECC can come up with the money.2 There have been other people infected by compounded drugs over the years but nothing as widespread as NECC. For many years, compounders were loosely regulated by the states. Now there is new US federal legislature that requires sterile compounding facilities who sell across state lines to register as an outsourcing facility with the FDA under 503b. Each of these registered facilities must be GMP (Good Manufacturing Practice) compliant just like a sterile drug manufacturer. This new law should help prevent another tragedy like NECC and is also creating awareness in Europe and around the world about the risks of compounding pharmaceuticals without regulation.
Why don’t healthcare facilities perform routine monitoring as a part of infection control?
The CDC published guidelines on Environmental Infection Control in 2003. These guidelines state that environmental sampling in the United States has declined rapidly since 1970 because there are no standards or data to show correlation between hospital acquired infections and contamination of surfaces or air. As a result, this guideline only advocates performing environmental sampling in the event of an outbreak, a research study, monitoring for a bioterrorism situation or ‘sick’ building, or quality assurance. This quality assurance sampling only includes new construction or a change in infection control practice. “Conducting quality-assurance sampling on an extended basis, especially in the absence of an adverse outcome, is usually unjustified”.3 This document provides some good information on methods; however, it needs to be revised to include new technologies. Many concerns with microbial sampling have also been overcome by ready to use solutions from vendors who sell to the pharmaceutical industry.
prevention of contamination is the key to producing quality products
The pharmaceutical industry believes that a highly contaminated environment will affect the quality of their products and impact patient safety. Rick Friedman from the FDA published an article in 2005 on case studies involving contamination in sterile drug facilities and clearly showed that prevention of contamination is the key to producing quality products.4 Should WHO and local hospital accreditation organizations generate some guidance and standards around routine environmental monitoring for healthcare facilities to establish better contamination control?
Prevent Contamination by Validating Cleaning and Disinfection Methods
The Human Microbiome Project showed that our bodies are made up of 1-3% microorganisms and we have 360 times more bacterial genes than human ones 5. In any environment, people are huge sources of microbial contamination. There have been many studies to show that there is good correlation between contaminated surfaces and infection. Dr. John M. Boyce (now retired from Yale-New Haven Hospital) has published papers and presented data from some studies. The methods to assess cleanliness and disinfection that he discusses are 1) Visual inspection; 2) Observation of housekeeper technique; 3) Fluorescent marker; 4) ATP bioluminescence; 5) Traditional culture methods. Even though highly soiled surfaces will typically have a higher microbial load, microbial contamination is still invisible and could still result in an infection. Cleaning a surface improperly can show no reduction in microbial contamination. Sometimes there is even an increase in colony counts6.
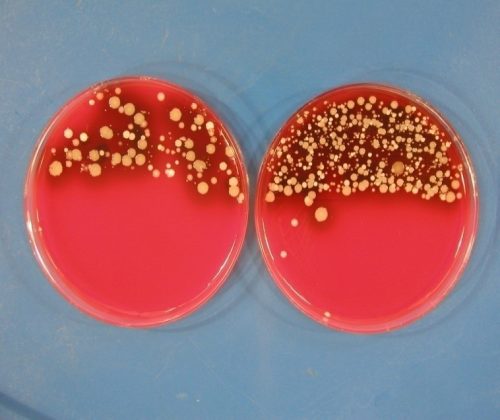
Overbed Table Overbed Table
Before Cleaning After Cleaning6
Observation and supervision have also proven to assist in reducing microbial contamination on surfaces but do not make microbial contamination visible. Both fluorescent markers and ATP swabs are good tools to assess microbial contamination but should still be compared against traditional culture methods to establish baseline as well as action limits in those environments. Even though culture methods require resources and time, they can still provide good comparison data for these new tools that provide immediate results. After determining the best approach to disinfection and cleaning through trial and error, one can establish an amount of contamination (such as the number of colonies per milliliter, or the quantity of ATP on the surface) that requires a corrective action. This corrective action could be an additional disinfection method followed by repeat monitoring to show that the contamination level has been reduced to an acceptable level.
One case study over a 21-month time period examined C. difficile contamination in isolation rooms. Phase 1 of the study utilized both fluorescent markers as well as training and feedback to housekeepers. Phase 2 added UV Disinfection and then Phase 3 included daily disinfection with rooms being cleared by a supervisor that used visual assessment and ATP indicators. The baseline demonstrated a 67% contamination rate with traditional culture methods while Phase 1 still showed 57%. Phase 2 decreased to 35% while Phase 3 dropped all the way down to 7%. It is very evident that a combination of cleaning and disinfection along with various monitoring methods can make a significant difference in contamination control7.
Let’s make some changes!
While it may be extreme to regulate hospitals like drug manufacturers, we may want to consider adopting some of these best practices such as validation of contamination control methods and routine monitoring. It simply is not enough to just have a contamination control program and a check list if a proactive approach is desired. Perhaps if standards and better guidance were written with pharmaceutical facilities in mind, we could create an increased awareness of microbial contamination and eventually reduce hospital acquired infections.
References:
- Eichenwald, K. Killer Pharmacy: Inside a Medical Mass Murder Case. newsweek.com; 2015. Available from: http://www.newsweek.com/2015/04/24/inside-one-most-murderous-corporate-crimes-us-history-322665.html.
- Judge Approves $200 million settlement over meningitis outbreak. (cbsnews.com); 2015. Available from: http://www.cbsnews.com/news/judge-approves-200-million-settlement-over-meningitis-outbreak.
- Friedman, R. Aseptic Processing Contamination Case Studies and the Pharmaceutical Quality System. PDA Journal of Pharmaceutical Science and Technology 2005; 59 (2): 116-126.
- Guidelines for Environmental Infection Control in Health-Care Facilities 2003, CDC.
- NIH Human Microbiome Project defines normal bacterial makeup of the body. (nih.gov).
- Principles of Environmental Cleaning and Monitoring the Adequacy of Practices. John M. Boyle, MD, Hospital of Saint Raphael. 06/15/2010.
- Monitoring Cleaning and Disinfection Practices. John M. Boyle, MD, Yale-New Haven Hospital. 12/2/2013.













[…] Protecting the Patient: Is it Time to Adopt Best Practices from the Pharmaceutical Industry? […]