Peer Reviewed
Abstract
This study focused on knowledge and practices towards bacterial vaginosis among non-medical students of Madonna University Elele. Four (4) objectives and four (4) research questions were used to guide the study. Related literature was reviewed and summarized. A descriptive study was used for the study. A sample of 100 female respondents were randomly selected for the study. The main instrument for data collection was a self-developed questionnaire. Data obtained and collected were presented and analyzed using descriptive statistics of frequency and percentage. The validity of the study was ascertained by other researchers while the reliability of the instrument was ensured through the test-retest technique, which yielded a positive correlation of 0.7. The results of the study revealed that a majority of the participants (75,63.0%) had the knowledge of bacterial vaginosis. It was also deduced that a majority of the respondents (64, 26.0%) believed that vaginal burning sensation is the most common symptom associated with bacterial vaginosis while few of the participants believed that foul odour could be the clinical manifestation of BV. Based on the findings, it was concluded and recommended that health education and enlightenment on BV should be done during school assemblies. One day per week scheduled for physical activity by female students, and weekly orientation can be used as an opportunity to enlighten students about hygienic health practices and BV.
Background
According to Centers for Disease Control (CDC) (2010), bacterial vaginosis (BV) is a polymicrobial displacement of normal lactociliary flora by anaerobic microorganisms, and is the most common cause of vaginal infection, characterised by an abnormal, greyish-white homogenous malodorous vaginal discharge (Forsum et al, 2010). Actual incidence and prevalence of bacterial vaginosis are unknown because up to 50% of women harbouring these abnormal bacteria are asymptomatic (CDC, 2010). Potter (2009) was of the opinion that women of any age are subject to bacterial vaginosis but women of reproductive age are more susceptible to the infection, with a reported prevalence ranging from 24% – 31.4%. Prevalence was higher in young girls and single women who tend to have more than one sexual partner (Potter, 2009). In Africa, the prevalence is very high in the sub-Saharan region, ranging from 30%-50% (Ankam and Reid, 2007). Ankam and Reid (2007) reported a rate of 14.2% for bacterial vaginosis among a population of Nigerian women, with the highest percentage occurring among Muslim and non-Catholic women. This was reportedly due to the frequent washing of the vagina with water after each micturition and the use of contraception respectively (Ankam and Reid, 2007).
In Madonna University, Nigeria, the rate of bacterial vaginosis is reportedly high among female students, due to practices which may predispose them to the condition, such as improper hygiene, wearing of ill-fitting underwear, having two or more sexual partners and use of harsh scented soaps to wash their vaginal area (Sari, Jaclyn, Kenneth., and Matthew. 2013). Bacterial vaginosis (BV) has been found to be associated with pelvic inflammatory disease (PID), significant reproductive morbidity (including premature rupture of the membranes and preterm delivery), and increased risk of HIV transmission (Payne et al, 2010 and Bilardi et al, 2013). Hence, timely therapeutic intervention and prevention strategies may decrease bacterial vaginosis-associated morbidity and the risk of HIV transmission. Therefore, it may be important to explore primary preventive strategies and knowledge about BV to prevent grievous health consequences.
Materials/Methods
A descriptive survey was used to study 100 randomly-selected female students, not in medical fields, between the ages of 16-24 at Madonna University Nigeria, Elele Campus. Participation was voluntary. A structured, validated questionnaire (see Appendix 1) was used as an instrument for data collection.
Results
DEMOGRAPHIC DATA
Table 1 : Description of participants
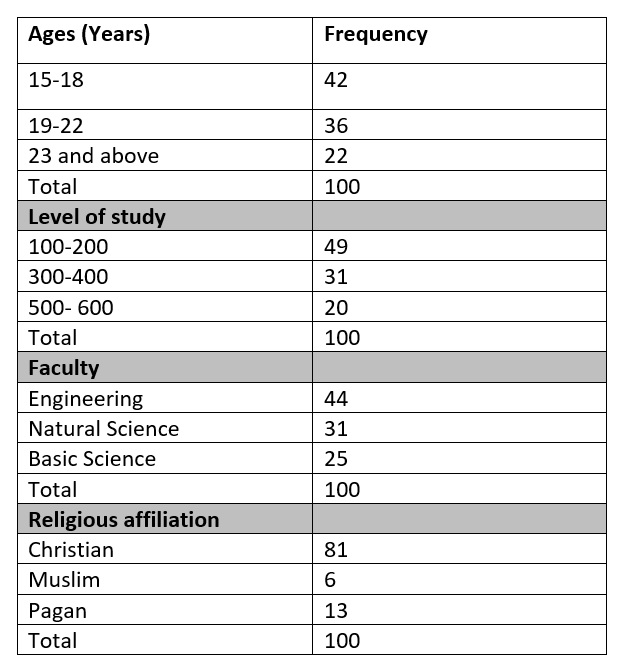
Table 1 shows the demographic data of respondents that participated in the study. A majority (42%) of the respondents were between the ages of 15 and18 years. Only 22% of the female students were above the age of 23 years. Of this population of female students, only 49% were in level 100-200 of their studies (first and second year university). Most of the study participants were either from the faculty of engineering (44%) or natural sciences (31%). A great majority of the respondents (81%) were Christian, and only 6% were Muslim.
KNOWLEDGE AND PRACTICE ASSESSMENT OF THE RESPONDENTS
Table 2: Knowledge Assessment on BV
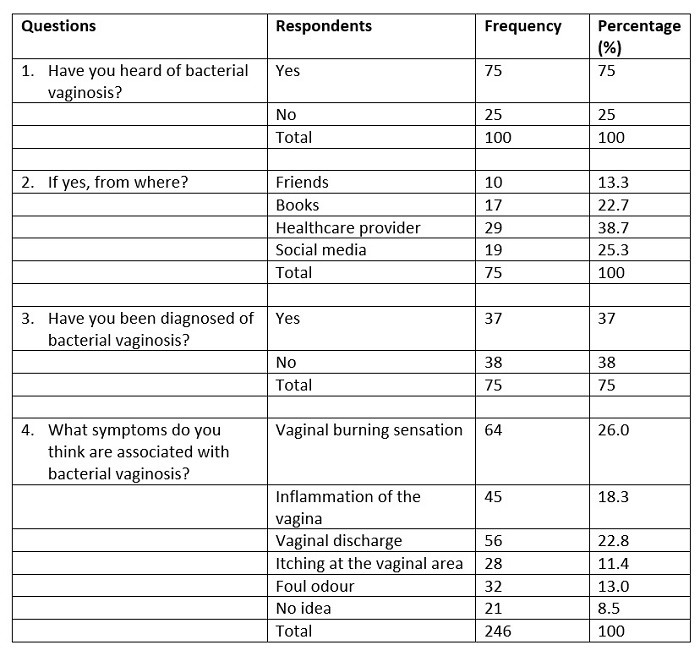
Table 2 presents the knowledge assessments of the respondents that participated in the study. An overwhelming majority of the participants (75%) had heard of bacterial vaginosis, with the main source of information being a healthcare provider (38.7%) or social media (25.3%). Only a small number of the participants had learned of BV from their friends (n=10, 13.3%). Of this population, 37% responded that they have been diagnosed with BV. The largest proportion of the respondents (26.0%) believed that vaginal burning sensation is the most common symptom associated with bacterial vaginosis. A number of of respondents (22.8%) also believed that vaginal discharge could be among the symptoms. Other signs and symptoms acknowledged by the respondents included: vaginal inflammation (45, 18.3%); itching at the vaginal area (28, 11.4%); and foul odour (32, 13.0%).
Table 3: Frequency distribution representing the practice assessment towards bacterial vaginosis.
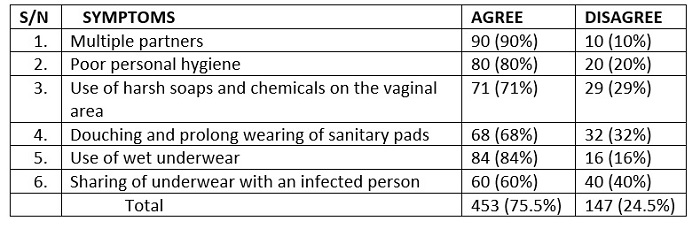
From the table above, it was observed that majority of the respondents (75.5%) were aware of the predisposing factors to BV. Of these, most of the respondents (90%) agreed that having multiple sexual partners could predispose one to BV. Other reported predisposing factors included: poor personal hygiene (80%); use of harsh soaps and chemicals in the vaginal area (71%); douching and prolonged wearing of sanitary pads (68%); use of wet underwear (84%); and sharing of underwear with an infected person (60%).
Table 4: Frequency distribution representing preventive measures towards bacterial vaginosis. (SA- strongly agree; A- agree; D- disagree; SD- strongly disagree).
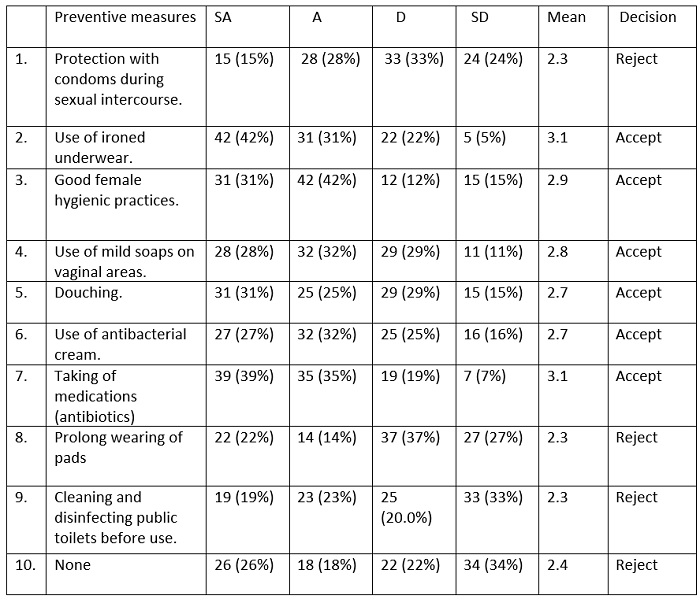
After assigning scores to each response (SA=4; A=3; D=2; SD=1), a mean score was calculated (2.5), which was used as a reference to determine which measures were most prevalent and could be evaluated as a preventive measure used by a majority of the respondents. Cumulative mean for each response was calculated. Cumulative mean scores of responses which were above the comparative mean were accepted, while scores below were rejected. The main preventive measures being practised by the female students were the use of dry underwear and taking of medications. Up to 73% believed that good female hygienic practices could prevent them from being contacted with BV. However, in opposition to clinical recommendations, most of the participants did not believe that prolonged wearing of sanitary pads (64%) and protection with condoms during sexual intercourse (57%) could be among the preventive measures of BV. Other preventive measures not commonly used among the female students were: cleaning and disinfecting public toilets before use; taking of medications (antibiotics); use of antibacterial cream; the use of mild soaps on vaginal areas; and douching.
Discussion
The study shows that many students not studying medicine were somewhat knowledgeable about BV. It was revealed that 75% respondents had knowledge of BV while 25% respondents did not. This was in contrary to a review by Marrzo et al (2012), who found that young girls, and especially university students, have a low level of knowledge and behavioural practices associated with BV. This group was more likely to engage in different forms of sexual activities without knowledge of the risk involved, and could contribute to the increase in BV cases worldwide, and especially in Africa. Payne et al (2010) also reported that knowledge of BV is low among young girls. In this study, of those who had knowledge about BV, 38.7% of them learned about it from healthcare providers. Nineteen percent of the respondents acknowledged that they have been diagnosed with BV. In previous studies it has been found that a majority of girls in Africa got knowledge about sexually transmitted diseases from their healthcare provider because of the perceived taboo associated with discussing sex-related issues, especially between parents and children (Marrzo, 2012; Jessica and Hemid 2016; Prakash 2016).
The most common BV symptoms acknowledged were vaginal burning sensation, with 64 (26.0%) of the respondents. Respondents could also identify other symptoms such as vaginal discharges, foul smelling odour, inflammation and itching on the vaginal area. Up to 8.5% of the respondents had no idea about symptoms of BV, of which 6.0% were between 15 to 18 years of age. In similar studies, the main symptoms that cause persons infected to seek medical advice was vaginal burning sensation (Eschenbach, 2007, Easmon et al, 2009, Baisly, 2013).
In this study, 75% of the participants were aware of at least one of the causes of BV. Senior students seemed to be more aware than students in their first two years in university. Of these respondents, 90% acknowledged that having multiple sexual partners could cause BV. According to Hillier (2010), frequency of BV in sexually active women had led to the proposal that BV is potentially sexually transmitted, however its pathology and transmission are still not completely understood. Some behavioral practices that may predispose women to BV include: sexual activities; frequent douching; use of scented harsh soap; use of deodorant products on the genitals; and change in sexual partners, among others (Hillier, 2010).
The main preventive measures of BV acknowledged amongst the participants included: good female hygienic practices (73%); use of mild soap on virginal areas (60%); douching (56%); use of anti-bacterial creams (59%); and taking of medications (74%). These findings agree with those of Bradshaw (2010), who proposed that these measures could help relieve symptoms of BV in women. However, methods such as the use of mild soaps on vaginal areas could increase the risk of contracting infections. It is recommended that maintaining good personal hygiene and using protection, such as condoms, during sexual intercourse should be highly recommended among the preventive measures against BV (Evans et al, 2007). According to Oduyebo (2009), douching may increase the risk of relapse of BV, however, there is no data to support the use of douching for treatment or relief of symptoms.
Recommendations
From the findings of the study, the following recommendations are proposed:
- Female students should be educated on personal hygiene practices, including the importance of keeping their environment and their toilets very neat and clean to avoid being contaminated with BV and being infected with other related diseases, like candidiasis, vulvovaginitis and trichomoniasis. Women with poor personal hygiene practices have been found to be more prone to BV infection (Melbourne Alfred Hospital Sexual Health Centre, Australia; 2016).
- There is a need for reproductive services in youth-based populations to help educate young girls on the dangers associated with BV and its prevention. Availability of friendly sexual and reproductive health services has been recommended by the United Nation Population Fund (UNFPA) for the promotion of adolescent sexual health and decrease in STI prevalence (UNFPA, 2014). Previous efforts have found a strong association between the availability of sexual and reproductive health services in Tanzania and the decrease in STIs (Richard, 2003).
- School administrators should liaise with hospital facilities and make available facilities and equipment towards appropriate screening and treatment of individuals to avoid complications, such as increased risk of sexually transmitted infections (STIs) and HIV. In an article on the benefits and risks of a screening test, it was found that its benefit is the control of epidemics of infectious disease. It also helps to target treatment of chronic diseases and reports of symptoms of lower genital tract infections (Udenze, et al, 2014)
- Health education and enlightenment on BV should be introduced during school assemblies. A day scheduled for physical exercise for female students can be used as a medium to enlighten students about hygienic health practices and BV. Health education has repeatedly been shown to have an impact on certain protective behaviours and on the frequency of sexual activity among students (Levy et al, 1995).
Conclusion
A majority of the population of female, non-medical students of Madonna University are of reproductive age and are more prone to BV compared to other ages (Potter, 2009). Knowledge about BV is high, whereas incidence is reportedly only 38%. Knowledge on preventive measures toward BV was fair. This was lower, as many students did not believe that methods such as disinfection of public toilets before use and protection with condoms during sexual intercourse could prevent BV. There is therefore a need for further health promotion among young girls and the public on how to reduce risk during sexual activity and practice proper toilet hygiene to help in the eradication of bacterial vaginosis among women (Sari et al, 2013; Marrazzo et al, 2010; Payne et al, 2010).
References
Akinsola, H.(2007). Research methods in medical and nursing practices. Ibadan: College press and publishers Ltd; 15-16
Ankam, K. and Reid. G. (2007). Organisms associated with bacterial vaginosis in Nigeria women as determined by PCR-DGGE and 16s RNA gene sequence. Nigeria: Africa Health Science. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1925267/
Baisly, K. (2013). Bacteria vaginosis in female facility workers in north-western. In sexually transmitted infection. North western Tanzania.
Bradshaw CS, Morton AN, Hocking J, Garland SM, Morris MB, Moss LM et al. 2006: High recurrence rates of bacterial vaginosis over the course of 12 months after oral metronidazole therapy and factors associated with recurrence. J Infect Dis. Available at https://www.ncbi.nlm.nih.gov/pubmed/16652274.
Richard Lord2003: Youth-Friendly Sexual and Reproductive Health Services: An Assessment of Facilities. Available at http://www2.pathfinder.org/site/DocServer/Youth_Friendly_Services_Summary_Assessment_Report_Tanzan.pdf
UNFPA(2014) Adolescent sexual and reproductive health. Available at ; http://www.unfpa.org/resources/adolescent-sexual-and-reproductive-health
Lawrence. A ., Obeagu E.I and Elemchukwu Q. (2014).Prevalence Of Bacterial Vaginosis Among Female Students Of Michael Okpara University Of Agriculture,Umudike, Abia State, Nigeria Udenze Chikwendu . Journal of Pharmacy and Biological Sciences. Available at Journal of Pharmacy and Biological Sciences
Bilardi JE, Walker S, Temple-Smith M, McNair R, Mooney-Somers J, Bellhouse Cet al (2013): The Burden of Bacterial Vaginosis: Women’s Experience of the Physical, Emotional, Sexual and Social Impact of Living with Recurrent Bacterial Vaginosis. Available at http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0074378
Prasanthi. I, CSE Goonewardena, Rasika Perera and RC Fernandupulle. (2015).
VAGINAL DISCHARGE: WOMEN’S HEALTH SEEKING BEHAVIOURS AND CULTURAL PRACTICES. Research Gate available at https://www.researchgate.net/publication/303384341_VAGINAL_DISCHARGE_WOMEN%27S_HEALTH_SEEKING_BEHAVIOURS_AND_CULTURAL_PRACTICES
Centre for Disease Control (2006). Sexually transmitted disease. Factsheet for STDS; Douching in relation to bacteria vaginosis, lactobacilli and facultative bacteria in the vagina. In obstetrics and gynecology.
Chris, F. (2006). Longman Active Study Dictionary. England: News gothic by Morton word processing Ltd.
Diana Rodriguez(2016). What Is Bacterial Vaginosis? Available at: http://www.everydayhealth.com/bacterial-vaginosis/guide/
Easmon C, Hay P, Ison C. Bacterial vaginosis: a diagnostic approach. Genitourin Med. 1992; 68(2):134–138. pmid:1582658
Evans AL, Scally AJ, Wellard SJ, Wilson JD. (2007): Prevalence of bacterial vaginosis in lesbians and hetero-sexual women in a community setting. Sex Transm Infect 2007, 83(6):470–475. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2598706/
Eschenbach DA.( 2007): Bacterial vaginosis: resistance, recurrence, and/or reinfection?. J. Clin. Infect.Volume 44. Available at https://academic.oup.com/cid/article/44/2/220/330015
Fethers K, Marks C, Mindel A, Estcourt CS: Sexually transmitted infections and risk behaviours in women who have sex with women. Sex Transm Infect 2000, 76(5):345–349. Available at https://www.ncbi.nlm.nih.gov/pubmed/11141849.
Jessica L. M and hamid Rushwan(2106): Adolescent sexual and reproductive health: The global challenges. International Journal of Gynecology & Obstetrics Volume 131. Available at. http://www.sciencedirect.com/science/article/pii/S0020729215000855
Marrazzo JM, Thomas KK, Agnew K, and Ringwood K (2010): Prevalence and risks for bacterial vaginosis in women who have sex with women. Sex Transm Dis. Pub Med available at https://www.ncbi.nlm.nih.gov/pubmed/20429087
Levy SR1, Perhats C, Weeks K, Handler AS, Zhu C and Flay BR (1995) Impact of a school based AIDS prevention program on risk and protective behaviour for newly sexually active students. Journal of school health. Available at https://www.ncbi.nlm.nih.gov/pubmed/7603052
Oduyebo. O, Anorlu RI and Ogunsola FT (2008). The effects of antimicrobial therapy on bacterial vaginosis in non-pregnant women. Cochrane Data based system revised (3). CD006055. Available at; https://www.ncbi.nlm.nih.gov/pubmed/19588379
Prakash Kanal( 2016): ADOLESCENTS KNOWLEDGE AND PERCEPTION OF SEXUAL AND REPRODUCTIVE HEALTH AND SERVICES- A STUDY FROM NEPAL. Available at http://epublications.uef.fi/pub/urn_nbn_fi_uef-20160398/urn_nbn_fi_uef-20160398.pdf
Payne S, Cromer P, Stanek M and Palmer A (2010): Evidence of African-American women’s frustrations withChronic recurrent bacterial vaginosis. J Am Acad Nurse Pract, Pub Med. 22:101–108. doi:10.1111/j.1745-7599.2009.00474. Available at https://www.ncbi.nlm.nih.gov/pubmed/20132368
Rosenstock, J. (1984). Health belief model. Theorist in nursing practice. 143›32-35.
Sally, W. &. (2008). Research Methodology. Oxford University press 13:4-5.
Sari L. R, Jaclyn M. W, Kenneth H., and Matthew J. M. (2013)Sexual risk
behaviors and psychosocial health concerns of female-to-male transgender men screening for STDs at an urban community health center. Pub Med doi: 10.1080/09540121.2013.855701 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4634528/
Sewankambo N, Gray RH, Wawer MJ, Paxton L, McNairn D, Wabwire-Mangen F et al: HIV-1 infection associated with abnormal vaginal flora morphology and bacterial vaginosis. The Lancet 1997, 350(9077):546–550.14.
Udontre, C. (2007). Basics of research and methodology (1st ed), Akwa Ibom: Emsel.
Women’s Management of BV and Experiences of Clinical Care PLOS ONE DOI:10.1371/journal.pone.0151794 March 24, 201612 / 13.
Appendix 1















