Abstract:
Antibiotics are almost single-handedly responsible for eliminating deaths and mortality caused by infectious disease. However, antibiotic resistance is disseminating among deadly pathogens, returning us to an era where death due to infection is a serious reality – the Four Horsemen of the Apocalypse are returning. To stay ahead of resistant infectious disease, we need to discover new antibiotics, judiciously use the antibiotics we have left, and ultimately understand the origin and evolution of antibiotic resistance.
Main Article:
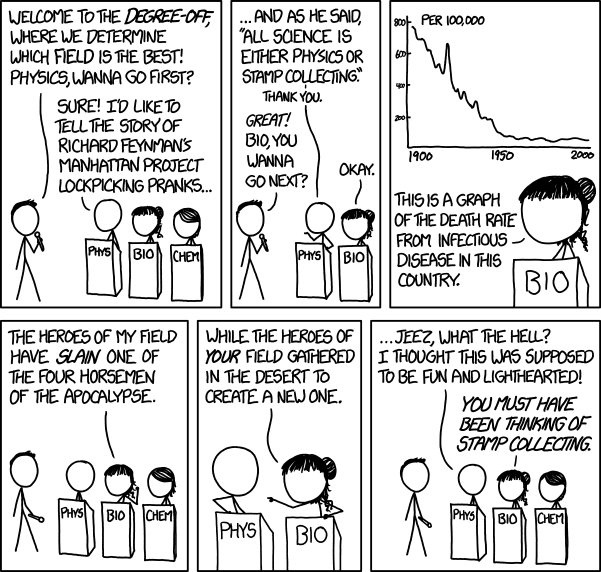
Antibiotics are among the most essential drugs available to medical experts to improve quality of life and eliminate unnecessary deaths due to infections. Antibiotics, in the traditional sense, are naturally produced substances that have anti-bacterial properties and are used in selective-chemotherapy – antibiotics inhibit bacterial cell growth without toxicity against human cells. Their discovery shifted medical treatments from invasive and dangerous surgical techniques to chemotherapy with relatively few side-effects and essentially eliminating the chance of dying from a common infection. This is in contrast to cancer chemotherapy where treatments are toxic to healthy cells while being more toxic to cancer cells. To paraphrase an xkcd comic, infection control and infection treatment basically eliminated one of the Four Horsemen of the apocalypse (Fig. 1). In 1900, infectious disease accounted for the top 3 causes of death and in 1998, pneumonia/influenza was the only the 6th leading cause of death (Fig. 2).
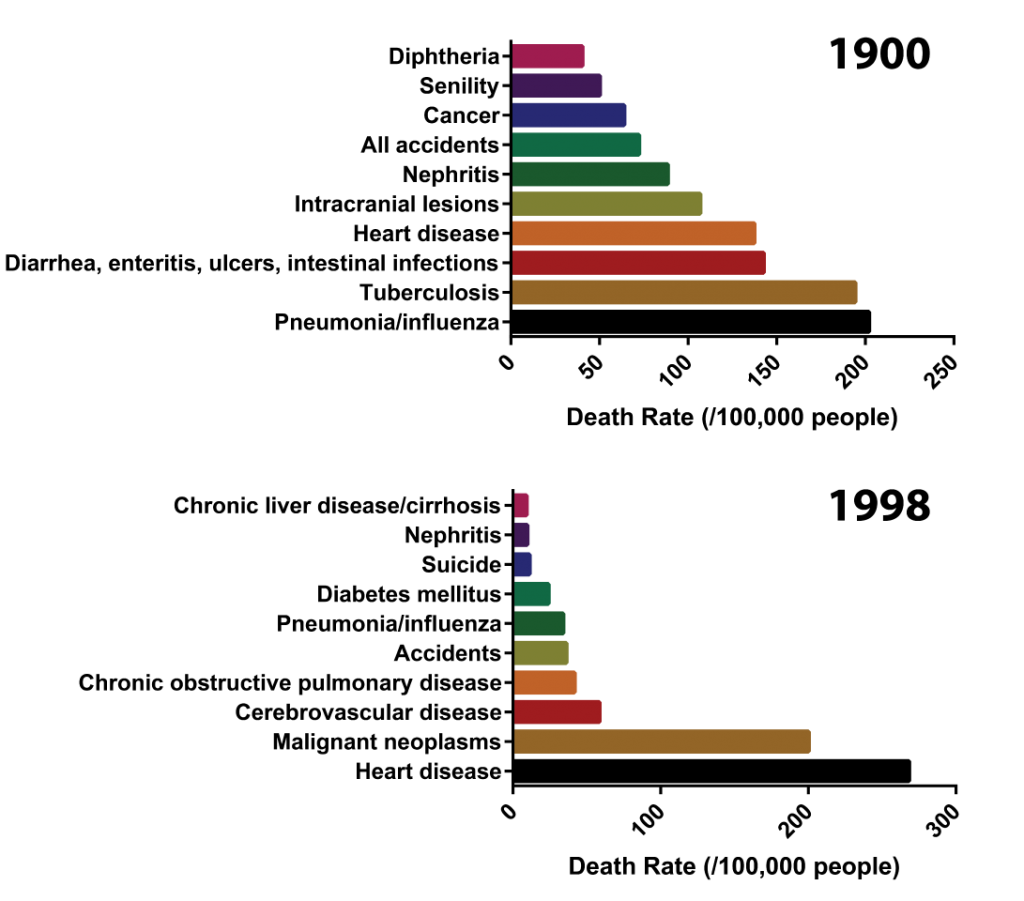
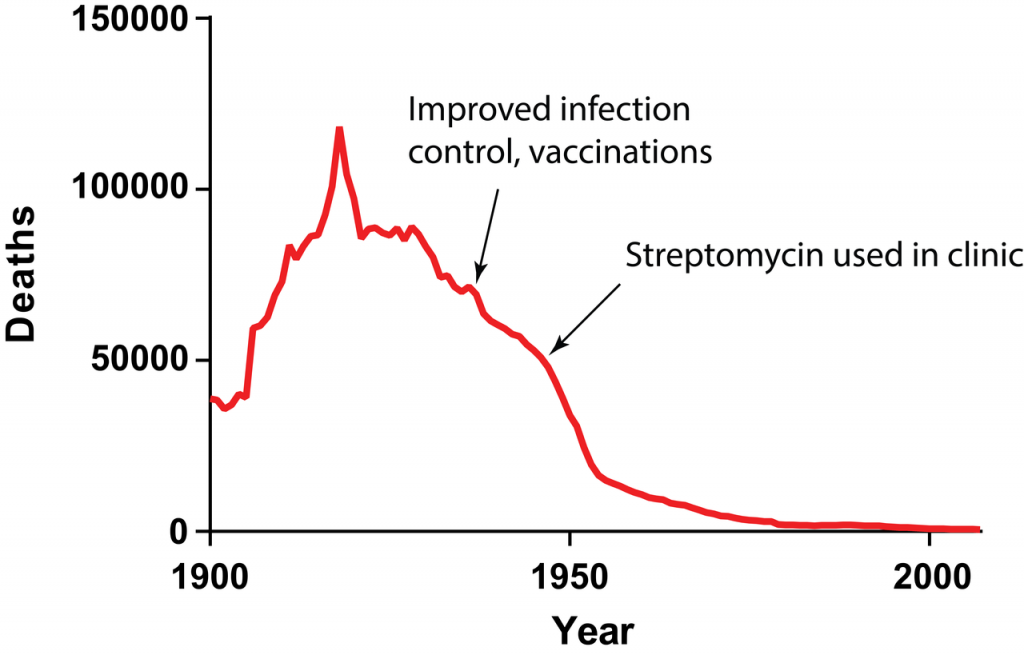
Tuberculosis was responsible for many deaths in the early 1900s’ (Fig. 3) and two of my great-grandparents died from tuberculosis. Infection control and the BCG vaccine was responsible for slowing the tide of deaths starting in the late 1920’s. Medical professionals could finally detect sick individuals in earlier stages of infection and quarantined these individuals to prevent the transmission of tuberculosis from person to person. Patients were being treated in sanatoriums which greatly increased the survival rate. However, the big break came in 1943 when Selman Waksman discovered streptomycin; the first antibiotic active against Mycobacterium tuberculosis, the causative agent of tuberculosis. He would go on to win the 1952 Nobel Prize in Physiology or Medicine for this discovery.
However, the Four Horsemen of the apocalypse are returning. Tuberculosis has acquired “resistance” – basically, it has learned/evolved in ways to prevent antibiotics from working. Drug-resistant tuberculosis is responsible for infecting millions of people in underdeveloped countries where infection control is limited and ineffective and access to lifesaving antibiotics is limited. Similarly, other pathogenic bacteria are acquiring resistance, many of which directly threaten us in first world counties. My Ph.D. supervisor became sick from a simple Salmonella infection and was not responding to the normal antibiotic regimen. After several weeks of hospitalization and after losing a large percentage of his body weight they were able to finally find an effective antibiotic to treat the infection. My childhood family doctor also almost died from a routine infection a number of years ago. He was only successfully treated with a state-of-the-art antibiotic. If this infection was to happen now, my family doctor may not have been so lucky; pathogens are now resistant to this state-of-the-art antibiotic.
We need to ask ourselves; are we really free from bacterial plagues? The answer is a resounding NO! Pathogens are routinely becoming resistant which limits the number of antibiotics that are still useful to treat infections. Even though I have been working in this field for ~7 years, I am only now confident that people are understanding the urgency in overcoming antibiotic resistance. Governments are finally allocating resources for research, and the WHO and CDC are emphasizing a potentially deadly future without antibiotics. We need to pressure governments to provide more money and to make sure it reaches the people who can have the most impact. We need new policies to limit unnecessary antibiotic use (e.g. in agriculture or placebo prescriptions for the common cold) and judicious management of the remaining effective antibiotics. We need to prioritize new antibiotic discovery, and not just slightly improvements on old drugs (which is why there are so many antibiotics with names that start with ‘cef-‘). And finally, we need to understand how resistance evolved and where it came from so that we can readily monitor infections and quickly react when new resistance appears.
Figure Legends:
Lead Image: Taken from http://freestock.ca/signs_symbols_g43-biohazard_grunge_sign__sepia_p1710.html under the Creative Commons License – Attribution 3.0 Unported
Figure 1: Infection control and prevention has slain one of the Four Horsemen of the apocalypse. Comic was taken from xkcd.com.
Figure 2: Infectious diseases are no longer the leading causes of death in the United States. The top 10 causes of death from 1900 and 1998 highlight the massive reduction of mortality from infectious diseases. Data obtained from the Center for Disease Control and Prevention (CDC).
Figure 3: The number of deaths attributed to tuberculosis infections in the United States between 1900 and 2007. Two events significantly improved the quality of life and decreased the mortality rate of infected patients; proper infection control (e.g. sanatoriums) combined with the BCG vaccine and the discovery and clinical implementation of streptomycin, the first antibiotic to treat tuberculosis.












