Abstract:
The CBS investigative news program “60 Minutes” aired a segment called “Strikethrough: A Matter of Life, Death, and Litigation” on Sunday May 1, 2016. Anderson Cooper reported that a major medical device and personal protective equipment (PPE) manufacturer may have hidden the truth about the ability of its products, specifically its Level 4 surgical gowns, to provide the right level of protection for healthcare workers on the frontlines in West Africa fighting Ebola Virus Disease. This article explores the risks associated with occupational exposure to infectious disease, specifically the importance of selection and use of PPE that is effective for certain biological hazards. It provides insights about whether the issue of strikethrough is based on real risk or whether it is just rhetoric used to create a newsworthy story.
Main Article:
On Sunday May 1, 2016, CBS aired a segment called “Strikethrough: A Matter of Life, Death, and Litigation” on its long standing, weekly investigative news program “60 Minutes”. In it, Anderson Cooper reported that a major medical device and personal protective equipment (PPE) manufacturer that was supplying surgical gowns to healthcare workers on the frontlines combating Ebola in West Africa may have hidden the truth about the ability of its products to provide the promised level of protection.
Personal Protective Equipment (PPE)
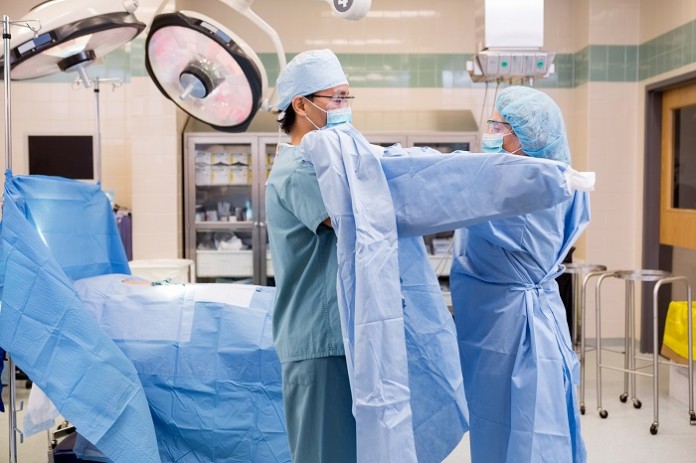
Healthcare workers rely on the use of PPE to protect themselves against infectious microorganisms. PPE use, compliance, and proper donning and doffing is especially crucial in times of crisis, like it was and will continue to be against the threat of emerging global infectious diseases like Ebola Virus.
Healthcare workers rely not only on the ability of the PPE they wear to protect themselves and their patients from cross-contamination and potential exposure to infectious disease, but also on the certainty that the PPE they are wearing is going to do as it says it will do; perform as it is marketed and labeled to perform; and protect them under the circumstance from which they need protection.
Failing to Protect
In Cooper’s segment, product testing failures from one major surgical gown manufacturer were called into question. These product failures may result in “strikethrough” which is a term used to describe the unintended penetration of a fluid, liquid, blood, or body fluid and the subsequent ability for the microorganisms in those fluids to get through the gown and onto the skin of the wearer.
To summarize what is a very complex issue, inter-laced with an intricate web of device design and engineering, manufacturing, supply chain, performance testing, and quality control systems, this manufacturer’s gowns failed to perform as indicated in many cases.
These surgical gowns – specifically ANSI/AAMI (American National Standards Institute/Association for the Advancement of Medical Instrumentation) Level 4 gowns – are worn to protect healthcare workers from the scariest of pathogens, like very small bloodborne viruses. This segment shed light on the fact that sometimes they do not work as promised.
While the segment focused only on exposures that occurred during surgery and in the operating room, this type of breach or failure of PPE, could also leave other workers exposed, including lab workers, researchers, emergency personnel, sterile processing personnel, environmental services staff, clergy and transporters.
A notable percentage of this manufacturer’s surgical gowns were failing performance testing in laboratory settings
A notable percentage of this manufacturer’s surgical gowns (ranging from 21-77% depending on test type) were failing performance testing in laboratory settings. In addition, the gowns were also failing to even stay intact during actual surgical procedures. Surgeon users indicated that, during their surgeries, sleeves would fall off, blood would soak through to their skin, and seams would rip and leak.
The Risk of Inadequate PPE
When blood or body fluids contaminated with an infectious disease touch non-intact skin or mucous membranes, there is a real risk that the exposed person could contract the disease. Given that healthcare workers are wearing scrubs under their gowns, the likelihood that infected fluids touch the torso or other more heavily protected areas is low. However, since surgical attire does not protect the arm, wrist, neck, or head, risk of exposure to those areas is higher, which is why workers rely on PPE to do that. In a long or physically intensive surgery, there is an enormous amount of movement, rubbing, friction, and stress on these areas, meaning that the ability for the PPE including gloves, cuffs, and sleeves to remain intact as a barrier is especially important.
One of the surgeons that was interviewed for the segment said that, at the end of one of her long procedures, she realized that she had worn off a callous on her skin , creating a high risk microbial entry point due to non-intact skin. Bloodborne viruses like HCV and HIV are especially worrisome during these types of occupational exposures. If PPE fails, this exposure could be life altering.
Occupational exposure incident surveillance data collected by EPINet® (Exposure Prevention Information Network) illustrates that not only are clinicians experiencing patient blood and body fluid exposure to skin (intact and non-intact), but also that exposures are occurring within gaps in protective clothing and even soaking through barrier garments, like surgical gowns.1 These types of exposure incidents, coupled with already low PPE compliance, exacerbate the danger of a situation.
ANSI/AAMI performance criteria for different levels of surgical and isolation gowns depend on hazard-based testing, to include varying degrees of impact penetration strength, pressure or velocity of liquid exposures, liquid particle size, liquid type (water, oil, synthetic blood), and cellular penetration (virus, bacteria, spore), among others.2 Testing conducted by National Institute for Occupational Safety and Health (NIOSH) last year, had already indicated that failing performance testing is not unique to only Level 4 gowns, but also to the more flimsy, disposable Level 1 and 2 varieties, which are used multiple times per day per clinician during routine procedures.3
Risk or Rhetoric?
Cooper interviewed the Chief Operating Officer of Halyard Health (the manufacturer or the gown), who said the company had a very low rate of complaints, and no reports of even one healthcare worker contracting an infectious disease due to a failure of its gowns. If the risk is relatively low for contracting an infectious disease through barrier garments and PPE, even when they fail, is this all just rhetoric?
No. With the onset of the AIDS epidemic in the 1980s and the subsequent roll out of universal and standard precautions, we long ago learned to assume that all blood and body fluids and all patients are potentially infected or ill with a pathogenic microorganism. This “blanket” theory of infection prevention practice ensures that we select the appropriate PPE for the risk and are continuously protected for the variability of everything else: the type and duration of procedure; the type and severity of the injury, illness, or treatment; the mobility or personal factors related to the patient; the location of care; the emergent or urgent nature of care; accessibility to other staff or specialists; etc.
Caring for patients, the community, and the public is hectic. It is uncertain. It is ever-changing. Global, and even local, threats are emerging or unknown. Protecting yourself is a constant.
Ultimately, Halyard Health is not likely the only PPE manufacturer with devices or equipment that fail in both laboratory and real-world settings. They are, however, a reminder that we, as advocates for safety, must hold manufacturing processes and quality systems to a higher level of accountability and effectiveness. We must work collaboratively with manufacturers to ensure that they know how their devices and equipment are being used and why we rely on them to perform.
This piece calls into question the manufacturing parameters of all products that we rely on to keep us safe to include, not just medical devices and PPE. Seat belts, baby seats, harnesses, fire retardants, motor vehicles and even electronics all need to be strictly regulated and rigorously tested so that we, as consumers, can be assured that a product that is marketed to do something as important as protecting us from harm, does just that.
The segment was reported by Anderson Cooper and produced by Andy Cohen and Sarah Fitzpatrick. A link for the segment is available online at: http://www.cbsnews.com/news/60-minutes-investigates-medical-gear-sold-during-ebola-crisis/
- International Safety Center. Exposure Prevention Information Network (EPINet) Summary Report for Blood and Body Fluids, 2013. http://internationalsafetycenter.org/wp-content/uploads/2015/08/Official-2013-BBFSummary.pdf
- National Institute for Occupational Safety and Health. Considerations for Selecting Protective Clothing used in Healthcare for Protection against Microorganisms in Blood and Body Fluids. http://www.cdc.gov/niosh/npptl/topics/protectiveclothing/
- Kilinc Balci, F. Selcen. Isolation gowns in health care settings: Laboratory studies, regulations and standards, and potential barriers of gown selection and use. American Journal of Infection Control, Volume 44 , Issue 1 , 104 – 111












Worth reading article. Medicine and medical sciences has been changing far over an era of time. The concerned tactics to deal with the medical history has been always a part and to describe its best use ancient methodology is always taken into consideration. Medical profession and the usage of scrubs is being more in trend today. The personal protective equipments are essential for medical personals to avoid risk factor. Thus scrubs like http://www.salusuniforms.com/ are the measures through which nurses and doctors can strikethrough the risk.