Staff culture eats strategy for lunch.
Or was it breakfast?
THIS OPPORTUNITY HAS CLOSED.
THANK YOU TO ALL THAT APPLIED.
This snappy phrase, often attributed to management guru Peter Drucker, is meant to suggest that culture often determines and very much limits strategic planning efforts in large organizations.[i] However, this does not seem to be a well-understood phenomenon in healthcare, particularly in hospitals. While some organizations are able to learn from mistakes and adapt in ways that improve quality, complex organizations, such as hospitals, are often unable to do so.[ii]
Over the past decade, hospitals have wrestled with improving safety and quality to prevent and control hospital-acquired infections. The fact is that many of these initiatives have failed,[iii] have been un-measurable, or have ignored clinical outcomes in favour of projects or campaigns that are easy to fall back on and to game (like trying to measure and improve hand hygiene).
Organizational dynamics and structures prevent improvement at multiple levels of analysis: the industry, the institution, and the department. Therefore, quality and safety interventions aimed at changing collective work practices are unlikely to be sustained beyond the intervention period itself. [iv]
To get at the root of the infection challenge facing a hospital, it is necessary to approach the culture of the hospital, on a unit-by-unit basis, to really understand what we’re all up against in designing and implementing strategy.
To this end, Infonaut has developed a Risk, Behavior and Culture Assessment that involves participating staff (ranging from doctors and nurses to imaging technologists and aides) taking a 75 question, online survey. The survey itself will takes about 15 minutes to complete.
This is the first step in an alternative approach, which focuses on psychological processes of the individual, rather than the normative behaviour of the group. Key psychological principles that govern the cognition, affect, and behaviour of individuals will be reviewed.
focuses on psychological processes of the individual, rather than the normative behaviour of the group.
The results of the survey will provide a foundation for quality and safety interventions, levering these principles to target specific behaviours among staff. A focus on the individual, rather than the group, can change patient safety behaviour on the hospital’s front lines.
Organizational culture enacts extreme resistance to efforts at changing policy and practice. However, a better model will draw upon a broad set of theories and principles concerned with changing the behaviour of the individual, rather than trying to redirect the herd. In contrast to efforts toward change directed at groups of people, when the right levers are used, individual behaviours can be highly receptive to change.
The survey and assessment will highlight the challenges the individual hospital faces in improving quality and safety and then, ultimately, highlight those interventions that will be the most successful, based on the culture of the unit.
Assessing Frontline Attitudes and Culture
Frontline clinical staff is invited to complete the Risk, Behavior and Culture Survey. We know your time is valuable, so we have built in an incentive to completing the survey: you will receive up to 1.25 hours of continuing education credits, if you are eligible, from a US or UK-based educational institution. These credits can be applied globally.
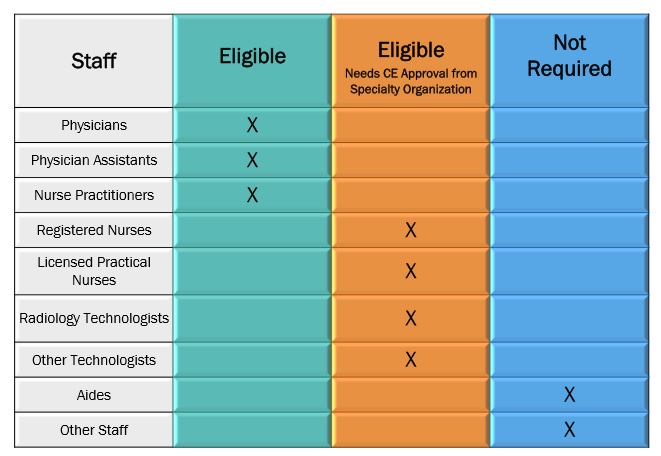 Free Continuing Education credits for eligible clinical staff that participate
Free Continuing Education credits for eligible clinical staff that participate
The purpose of this survey instrument is to learn about clinical staff perceptions of their information use habits and norms, and perceptions of patient safety and the role of management.
Results may be used to identify both obstacles and opportunities for introducing specific interventions on a unit-by-unit basis, provided that enough unit-level staff participate.
The survey specifically measures:
- Unit attitudes to patient safety;
- Unit capacity-to-learn as a group;
- Unit information culture; and
- Personal perception of risk.
Typically, the results of these measures will be presented to staff, and can act as a baseline measure for interventions targeting staff attitudes and dynamics. Follow-up retesting after a set period (e.g. one year) will help determine if there is a measureable change in culture based on the effective interventions and relationships that result.
results of this survey will be published here, on the TIPS Journal
The results of this survey will be published here, on InfectionControl.tips and will be presented at the Infection Prevention & Control 2016 Conference in Manchester, England on September 6, 2016.
We invite frontline staff to participate ANONYMOUSLY and help us identify the challenges facing hospitals globally. By doing so, you will help determine the most appropriate steps to take to enact the change needed to improve patient safety.
THIS OPPORTUNITY HAS CLOSED.
THANK YOU TO ALL THAT APPLIED.
References:
[i] George Anderson, QUORA – https://www.quora.com/Did-Peter-Drucker-actually-say-culture-eats-strategy-for-breakfast-and-if-so-where-when – as viewed on June 30, 2016
[ii] United States Government Accountability Office (GAO) – Patient Safety: Hospitals Face Challenges Implementing Evidence-Based Practices February 2016http://www.gao.gov/assets/680/675390.pdf
[iii] Binder, Leah, President and CEO of The Leapfrog Group – Forbes Online March 15, 2016 http://onforb.es/1RiTstN
[iv] Dixon-Woods, et al. Ten challenges in improving quality in healthcare: lessons from the Health Foundation’s programme evaluations and relevant literature BMJ Qual Saf 2012;21:876-884 doi:10.1136/bmjqs-2011-000760












