Abstract:
The use of hand sanitizers is ubiquitous in public places all over the United States. Although this promotes better hand hygiene, improper use renders many of these dispensers useless.
Main Article:
Proper hand hygiene plays a pivotal role in any successful infection prevention program as well as our overall good health. Numerous studies show that many people are not washing their hands correctly, or not at all (Boshell, 2015). Yet everywhere I go I see the ubiquitous hand sanitizer. This is a good thing. But has this advancement in infection control made people more complacent about simply washing their hands with soap and water when they can get foam or gel squirted on their hands automatically? Hand sanitizers have revolutionized how we can easily disinfect our hands on the go, but hand washing does have its time and place. They should work in concert with each other, to have truly clean hands.
Hand sanitizers have revolutionized how we can easily disinfect our hands on the go
“Nosocomial infections (an infection that is acquired in a hospital) occur in the U.S. about 2 million times annually” (Kampf, 2004). These 2 million patients went to the hospital because they were sick enough to be there, and while there, acquired another problem. It should be noted that as the U.S. population ages, we will see older patients with more comorbidities as patients in hospitals. Older patients are simply just more vulnerable to infections in a hospital. The patients in hospitals today are vastly different than 20 years ago. More and more people have multiple health issues such as congestive heart failure, kidney failure, diabetes, and Legionellosis, concurrently! This is not out of the ordinary. These patients are fragile and already at risk. It is our responsibility to take extra care of these patients. Tetro (2015) stated “it’s up to the individual to be responsible and follow the guidelines.” Shouldn’t we be diligent in our actions when treating them so they don’t acquire a new problem they have to fight?
“Healthcare workers’ hands are the most common vehicle for the transmission of healthcare-associated pathogens from patient to patient and within the healthcare environment” (Allegranzi, 2009). In this environment, the health care workers act as a vector for transmission of infection. Common nosocomial infections include: central line-associated bloodstream infections, catheter-associated urinary tract infections, surgical site infections, and ventilator-associated pneumonia. The most common nosocomial pathogens are Staphylococcus aureus, and Methicillin resistant S. aureus (MRSA), Clostridium difficile, E. coli, Vancomycin-resistant Enterococci (VRE), Vancomycin-intermediate S. aureus (VISA), to name a few. Some of these commonly transmitted pathogens are also happen to be on the top of the list for being resistant almost all antibiotics, or extremely hard to eradicate like C. difficile spores.
The adoption of alcohol-based hand rubs is considered the gold standard for hand hygiene in clinical settings
“The adoption of alcohol-based hand rubs is considered the gold standard for hand hygiene in clinical settings” (Allegranzi, 2009). This standard is backed by the CDC and WHO for its ease of use, efficiency, and effectiveness in killing gram negative bacteria “that make up approximately 64% of nosocomial infections, gram positive bacteria that make up approximately 15% of nosocomial infections, fungus, some viruses, about 5%” (Kampf, 2004).
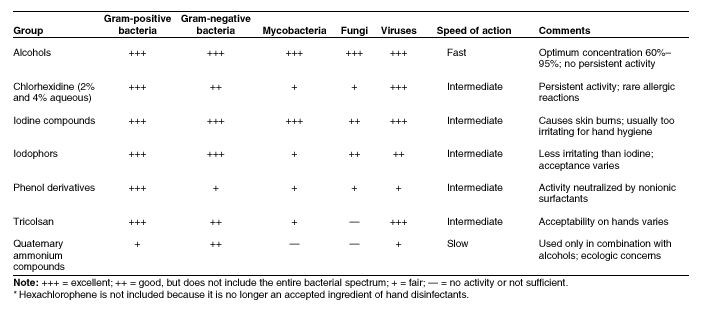
The above chart compares hand hygiene antiseptic agents against microorganisms, speed of action, and a note about each. Looking at this, one can see that alcohol based hand sanitizers outperforms all other antiseptic agents that are in use. But some people are a little skeptical about using them. There remains a few myths about what they are and what they do.
Let’s do a little Q & A:
- Hand sanitizers can replace washing with soap and water?
- Hand sanitizers are less effective than soap and water?
- Is hand sanitizer toxic?
- Will they kill everything?
- Are teens misusing this product?
Did you answer No for questions #1-4 and yes for #5? If yes, great job! If no, keep reading. Hand sanitizers should be used in place of hand washing with soap and water. Normal hand washing is needed for visibly soiled hands. The friction of washing and drying with a paper towel remove the layer of “grime” from hands so that hand sanitizers can work effectively. If there is no access to soap and water, then this should be the alternative to doing nothing. Hand sanitizers are good for one thing- sanitizing. They are not cleaners of hands, per se. This is why we recommend washing first. “Sanitizers will not be able to penetrate through a layer of grime. That must be removed first” (Barnett, 2013). “The most effective hand sanitizers contain between 60-95% ethyl alcohol” (Kampf, 2004). You do not want to use 100%, as the alcohol works the best with a little bit of water in the solution. While alcohol-based sanitizers are the “gold standard”, certain formulations use the antibacterial chemical triclosan. Triclosan is an antibacterial agent that is used in non-alcohol-based sanitizers. “There’s no good evidence that triclosan-containing products have a benefit … When you expose bacteria to triclosan, it can elicit antibiotic resistance” (Barnett, 2013). Antibiotic resistance is one of the most pressing public health concerns worldwide. Looking at the different hand hygiene antiseptics below, we see that alcohol-based ones are effective at killing all groups of microorganisms quickly. There are one or two caveats though. They will not kill bacterial spores (C. difficile) and certain non-enveloped viruses (Norovirus) . These need the mechanical action of hand washing and rinsing to remove. It has been suggested that using hand sanitizer after washing will make your hands unwelcoming to Norovirus.
Read More:
Liberia: Dangerous Soap Slurry to Clever Drying Hooks
https://infectioncontrol.tips/2015/12/01/liberia-soap/
Patient Hand Hygiene: The missing link in preventing Hospital Acquired Infections?
https://infectioncontrol.tips/2015/12/09/patient-hand-hygiene-the-missing-link-in-preventing-hospital-acquired-infections/
Building a Career In Infection Prevention: Jomcy’s Story
https://infectioncontrol.tips/2015/11/13/building-a-career-in-infection-prevention-jomcys-story/
Hand Hygiene Nigeria: Implementation Lessons
https://infectioncontrol.tips/2015/11/13/hand-hygiene-nigeria-implementation-lessons/
Is the Flu (or another bug) on Your Menu Today?
https://infectioncontrol.tips/2015/11/26/1080/
References:
Allegranzi, B., & Pittet, D. (2009). Role of hand hygiene in healthcare-associated infection prevention. Journal of Hospital Infection, 73(4), 305-315.
Barnett, Bob. (2013) Is Hand Sanitizer toxic? Accessed 11/11/15 CNN.com
Berkeley Wellness. (2014) 6 Things About Hand Sanitizers. Accessed Nov. 11, 2015
http://www.berkeleywellness.com
Boshell, P (2015) 5 Gross Hygiene Facts. Accessed Dec 7, 2015
http://info.debgroup.com/blog/5-gross-hygiene-facts/
CDC. MMWR October 25,2002/ 51 (RR16);45
Draelos, Zoe Diana. (2013) Which Hand Sanitizers are the most practical and effective? Accessed Nov. 11, 2015
http://dermatologytimes.modernmedicine.com
Dunn, Rob. (2011) Scientists Discover That Antimicrobial Wipes and Soaps May Be Making You (and Society) Sick. Accessed Nov. 11, 2015 http://blogs.scientificamerican.com
Infection Control Today: Surface Disinfectants. (2015) Accessed Nov. 11, 2015 http://www.infectioncontroltoday.com
Johns Hopkins Medicine. WIPES Infection Prevention Program and Cleaning Your Hands. Accessed Nov.11, 2015 http://www.hopkinsmedicine.org
Kampf, Gunter & Kramer, Axel. (2004). Epidemiologic Background of Hand Hygiene and Evaluation of the Most Important Agents for Scrubs and Rubs. Clinical Microbiology Reviews, 17(4) 863-893.
Penn Medicine. Hand Sanitizer- The Facts, the Myths and What Your Teenage Might Be Doing with it. Chester County Hospital.(2012). Accessed Nov.11, 2015 http://www.cchosp.com
Saloojee, H & Steenhoff A. The Health professional’s role in preventing nosocomial infections. Postgraduate Medical Journal. 2001;77:16-19.
Tetro, J (2015) Where There’s a Will, There’s a Way. Accessed Dec 7, 2015
http://info.debgroup.com/blog/where-theres-a-will-theres-a-way/
Todd, EC. Outbreaks where food workers have been implicated in the spread of foodborne disease. Part 10. Alcohol-based antiseptics for hand disinfection and a comparison of their effectiveness with soaps. Journal of Food Protection. 2010. Nov; 73(11):2128-40.













Good article Lisa,
Maybe we should also consider the materials used for the product dispensers, in particular the frequently-touched areas. In an ideal world (and per supplier instructions) these units should be cleaned frequently and the contents changed within a specified time period, whether finished or not). However, compliance varies and microbial contamination is not always visible to users / patients / visitors.
There are several papers regarding pathogen survival on standard clinical surfaces, including plastics, and an increasing body of evidence affirming the intrinsic antimicrobial properties of metallic copper & copper-alloys (collectively called “Antimicrobial Copper”).
Of particular interest is the ‘real-life’ rapid efficacy of Antimicrobial Copper surfaces, under typical indoor conditions, against bacteria (gram+ve and -ve), viruses (enveloped or not), yeasts and fungi (including spores).
We look forward to an appropriate test protocol to measure antimicrobial efficacy pertaining to touch surfaces, as the limitations of ISO 22196 and JIS Z 2801 are becoming better know.
This recent paper, published in HERD, helps summarise and explain the mechanisms, efficacy, benefits and payback of Antimicrobial Copper surfaces:
Michels HT, Keevil CW, Salgado CD, Schmidt MG. 2015.
From Laboratory Research to a Clinical Trial: Copper Alloy Surfaces Kill Bacteria and Reduce Hospital-Acquired Infections
HERD, October 2015 vol. 9 no. 1 64-79, doi: 10.1177/1937586715592650
http://her.sagepub.com/content/9/1/64
Use of Antimicrobial Copper is recommended as an adjunct to, and not a substitute for, good hand hygiene and cleaning regimes.
Truthfully soap and water have no replacement or alternative to have good hand hygiene. In our study a few years back we found that surgeons have highly drug resistant bacteria on their hands and due to false assurance provided by the sanitizers they keep on spreading the diseases. You may see our publication at:
https://www.researchgate.net/publication/258831612_Carriage_of_Carbapenemase_Resistant_MDR_Strains_of_Acinetobacter_Baumannii_and_Staphylococcus_Carnosus_on_Hands_of_Surgeons_in_Bareilly_India