Abstract:
Background: More people in the US now die from Methicillin-Resistant Staphylococcus aureus (MRSA) infections than from HIV/AIDS. Often acquired in healthcare facilities or during healthcare procedures, the extremely high incidence of MRSA infections and the dangerously low levels of literacy regarding antibiotic resistance in the general public are on a collision course. Traditional medical approaches to infection control and the conventional attitude healthcare practitioners adopt toward public education are no longer adequate to avoid this collision. I conducted a study with MRSA survivors using constructivist theory, semi-structured face-to-face and phone interviews which allowed participants to tell their stories so their experiences could deepen our understanding of this crucial health issue.
Significance: This study underscores the critical importance of educational programs for patients, and improved continuing education for healthcare providers. Five specific results of this study can reduce the vacuum that currently exists between the knowledge and information available to healthcare professionals, and how that information is conveyed to the public. These points include: 1) a common model of MRSA patients’ learning and adaptation; 2) the self-directed nature of adult learning; 3) the focus on general MRSA information, care and prevention, and antibiotic resistance; 4) the interconnected nature of adaptation; and, 5) the need for a consistent step by step plan to deal with MRSA provided at the time of diagnosis.
Main Article:
Over the course of my public health, clinical, and academic career, I have had the opportunity to be part of both national and international efforts for a variety of “headline” outbreaks of both animal and human infectious disease. While working as a microbiologist and virologist for the Texas Department of State Health Services (DSHS), I had the honor of being with the initial team of scientists to conduct the Oral Rabies Vaccination Program to eliminate canine rabies from Texas.1-4 This international effort was the foundation for creating my outlook on the importance of health education surrounding efforts to inform the general public about sometimes complex (and often scary headlines) infectious diseases. Over the course of a decade with the DSHS and some short stints as a visiting scientist with the CDC, I helped in both laboratory and general public health facets for Rabies, West Nile Virus, Hantavirus, Anthrax, Yersinia pestis (plague), and many others that one sees come and go in the popular press.
After transitioning to the world of academia at Texas State University in 2002, I continued with my public health endeavors with these microbes and others. However, after conducting a research study on methicillin-resistant Staphylococcus aureus (MRSA) in correctional facilities (prison)5 in 2006-07 my outlook completely changed due to the global problem of antibiotic resistance. I began to receive phone calls and emails, often from complete strangers, in regards to this “MRSA” problem that seemed to be amplifying and spreading like wildfire in certain populations – especially healthcare. These people were desperate for help and advice that they were not getting from their physicians or (Staphylococcus aureus) and MRSA issues. It was at that moment that I realized what my dissertation for my PhD would be – Stories from MRSA survivors and what they needed others to understand about this global epidemic of Healthcare Associated Infections (HAIs) like MRSA.6,7
MRSA first emerged as a serious infectious threat in the late 1960s as the bacterium developed resistance to the synthetic form of penicillin known as methicillin.8 Although the Staphylococci bacteria, including MRSA, commonly colonize the skin of healthy people, often posing little to no threat, these bugs are quick to exploit any opportunity to invade wounds, nasal passageways, or mucosal membranes where they can rapidly produce infections that can become life threatening. It is not surprising then, that MRSA has been the focus of intense scientific and political interest around the world9,10 and has frequently been labeled as a superbug in the popular media.11
As the number of MRSA infections acquired both within healthcare facilities and, more recently, in community settings that bring large numbers of people into close proximity have increased, research has begun to focus on levels of public awareness and misperceptions connected with MRSA. In particular, this decade has produced a number of significant studies in the United Kingdom and Europe that have investigated public perceptions and the role played by the popular media as purveyors of information. As recently as 2006, a study conducted in the UK12 found that 68% of the lay people they surveyed acquired their knowledge of MRSA from a combination of television and newspapers. An earlier qualitative study reported a lingering level of confusion in patients being treated for a MRSA infection, that persisted even after information about the infection had been provided by healthcare professionals.13 These findings are further supported by a 2007 investigation into public awareness and attitudes which reported “the media [continues to act] as a conduit between medical and lay knowledge and . . . is the main source of public information about resistant infections.”14 Finally, in perhaps one of the largest empirical studies of MRSA to date, conducted in the UK, researchers found that misperceptions surrounding MRSA tenaciously persist. This 2009 survey of 1,000 respondents found higher levels of public awareness than anticipated, and noted the primary source of information continues to be the media. But, perhaps most notable, the researchers report that “no one in [their] sample mentioned the contributions to MRSA of antibiotic prescribing by doctors or patient use of antibiotics.”11
The study I conducted and published delves deeper into the learning experiences of people who have lived through a MRSA infection in order to improve the practical management and outcomes of this disease. The complete study and results are very important, including a “Model of MRSA learning and adaptation, and can be found as an open access article with BMC as well as a published book.6,7 However, after all of the analysis and understanding, there is one important and practical message that I want to share with the world.
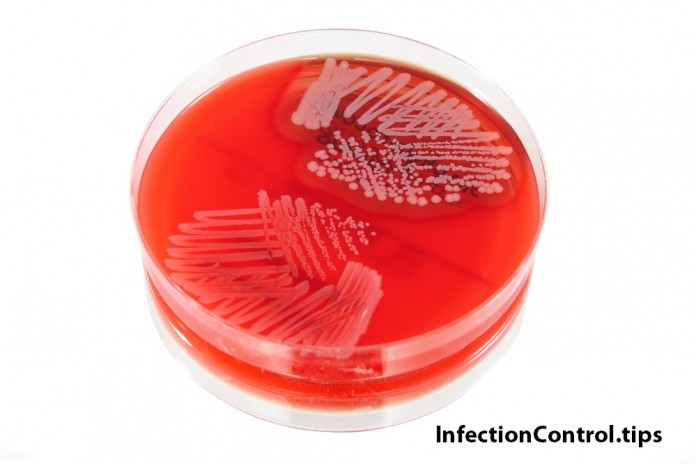
A MRSA diagnosis MUST BE based on A laboratory culture / Identification and antibiotic susceptibility testing!
Practice:
Current patient education programs about antibiotic resistant infections need to be revised. Particular attention should be paid to the following areas: a) the patient-healthcare provider interaction should intentionally cultivate an open and non-threatening environment to facilitate learning; b) the delivery of critical information about the importance of having a MRSA diagnosis based on laboratory culture and antibiotic susceptibility testing; c) specific education on what a MRSA infection looks like, including images/pictures and MRSA stories for patients; d) the use of social media, podcasts, digital video, and other electronic media to provide patient education beyond the initial MRSA diagnosis; e) specific education about infection care, control, and prevention to themselves and others; and, f) guidance for individuals about sources of information and the credibility of sources.
Without a laboratory confirmed diagnosis, physicians or others are just guessing!
These two tests – a culture/ID and susceptibility test – accurately identifies the bacterium that is causing the infection AND the correct antibiotic(s) one must prescribe to correctly treat the patient. It is critical to get this right the first time. If a physician or other uses an empirical, educated guess based on signs/symptoms or their “gut feeling” based on experience, they may be right. They could also be completely wrong. I suggest getting it right the first time. Of course, in cases of emergencies like sepsis, a physician may have to prescribe empirically by using a broad spectrum drug. But, they should still immediately follow up with a laboratory confirmation, period. Otherwise, the diagnosis is a guess, at best. Additionally, if you as a patient are intimidated by a physician or other to demand these tests, then bring an advocate with you to help. Educate yourself using reputable resources, and share it with any and all.
Final Thoughts:
I walk a hybrid path as a scientist who has and continues to conduct studies in regards to MRSA prevalence in people, animals, environment, as well as other projects. However, in the past five years I have found that my most important work may be my role as a translational researcher who continues to educate the general public (and other niche populations) about complex topics such as antibiotic resistance, HAIs like MRSA, zoonotic disease like Ebola, and other important public health issues. While some things like Ebola garner headlines, HAIs kill up to 300 people per day now. This is equivalent to a jet airliner full of passengers going down every day! Maybe we should all pay attention to what’s happening every day in our own backyard.
With regards to MRSA, I feel particularly dedicated because of my interaction with the people I’ve interviewed and advised (including my family and friends). It is with this knowledge that I often tell my students (future medical laboratorians and nurses), family, and the general public that if you do nothing else when a physician or other healthcare worker prescribes you an antibiotic empirically or tells you it’s “just a regular staph infection,” be sure to DEMAND a culture/ID and antibiotic susceptibility test. It just may save your life or that of a loved one!
References:
- Rohde, R.E., et al. 1997. Molecular epidemiology of rabies epizootics in Texas. J Clin Virol. 8:209-217.
- Sidwa, T., R.E. Rohde et al. Evaluation of Oral Rabies Vaccination Programs for control of rabies epizootics in coyotes and gray foxes: 1995-2003. J Am Vet Med Assoc 2005;227(5):785-792.
- Rohde, R.E. May, 2008. Controlling Rabies at its Source: The Texas Experience – Oral Rabies Vaccination Program. ASCLS Today, 22(5), 14-15.
- Wilson, P.J. & Rohde, R.E. 8 things you may not know about rabies but should. Elsevier Connect, September 28, 2015. http://www.elsevier.com/connect/8-things-you-may-not-know-about-rabies-but-should Accessed January 9, 2016.
- Felkner, M., R. E. Rohde, et al. Methicillin Resistant Staphylococcus aureus Nasal Carriage Rate in Texas County Jail Inmates. Journal of Correctional Health Care, 2007;13(4): 289-295.
- Rohde, R.E. et al. MRSA model of learning and adaptation: a qualitative study among the general public. BMC Health Services Research, 2012, 12:88. Accessed January 9, 2015.
- Rohde, R. E. 2011. Methicillin Resistant Staphylococcus aureus (MRSA) Knowledge, Learning, and Adaptation: I guess everything changes when it happens to you – their stories. LAP Lambert Academic Publishing GmbH & Co. KG, Dudweiler Landstraße 99, 66123 Saarbrücken, Germany. ISBN 978-3-8433-8225-0
- Washer P, Joffe H. The “hospital superbug”: Social representations of mrsa. Soc Sci Med 2006, 63:2141–2152.PubMedView Article
- Invasive mrsa. http://www.cdc.gov/ncidod/dhqp/ar_mrsa_Invasive_FS.html Accessed January 9, 2016.
- Darzi A.Z. Our nhs our future: Nhs next stage review interim report. London: Department of Health; 2007.
- Easton P.M., et al. A survey on public knowledge and perceptions of methicillin-resistant Staphylococcus aureus . J Antimicrob Chemother 2009, 63:209–214.PubMedView Article
- Gill .J, et al. Methicillin-resistant Staphylococcus aureus: Awareness and perceptions . J Hosp Infect 2006, 62:333–337.PubMedView Article
- Newton J.T. Patient’s perceptions of methicillin-resistant staphylococcus aureus and source isolation: A qualitative analysis of source-isolated patients. J Hosp Infect 2001, 48:275–280.PubMedView Article
- Hawkings N.J., et al. Public attitudes towards bacterial resistance: A qualitative study. J Antimicrob Chemother 2007, 59:1155–1160.PubMedView Article












Thank you for this important update Dr.
[…] Medical laboratory testing is the most critical component to a patient’s medical outcome, including the diagnosis of an antibiotic resistant infection. In fact, I preach to my students, colleagues, and anyone in healthcare or the general public that there are two things I want them to remember if they believe they have an infection. First, ask (or demand) that your physician order a diagnostic confirmatory laboratory test to identify your infection before they prescribe you an antibiotic, whenever possible. In most cases, no one (not even your physician) can tell you with certainty that you have a bacterial infection without a confirmatory laboratory test. You may have a viral illness, an allergy, or some other type of immune reaction that is NOT being caused by a bacterium. If you do not have a bacterial infection, an antibiotic is wrong for you. Second, IF you do have a bacterial infection, then be sure the provider orders an antibiotic susceptibility test when possible. This complex laboratory test will determine the susceptibility profile for the bacteria. It is JUST AS IMPORTANT as finding out you have a bacterial infection because it will let the physician and pharmacist know exactly which antibiotic(s) to use. Without this information, we are all just driving the issue of antibiotic resistance and superbug creation via “survival of the fittest!” These are two medical laboratory tests you must demand! […]