Abstract:
Diabetic foot infections are common and preventable occurrences that raise the risk of amputation. Regular foot screenings by a primary care physician are a first line of defense against such infections and can be life- and limb-saving. Simple self-care strategies also can help alert patients—particularly those with diabetic neuropathy—to foot lesions that may become infected, prompting them to seek appropriate care.
Main Article:
Background
Diabetic foot infection, defined as “a soft tissue or bone infection below the malleoli,” is the most common complication of diabetes that leads to hospitalization and the most frequent cause of nontraumatic lower extremity amputation (Gemechu et al., 2013). Research has shown that diabetic foot ulcers—open sores or wounds that don’t heal or heal very slowly and easily become infected—are preventable (American Podiatric Medical Association). Yet too few people with diabetes receive preventive care or take some simple steps on their own to help prevent infection.
The Problem
Regular foot screenings can be lifesaving for patients with diabetes. They are often the first line of defense against foot ulceration and infection, particularly when diabetes and/or concomitant vascular conditions cause loss of sensation in the foot (diabetic neuropathy) (Singh et al., 2005). Yet an Institute for Preventive Foot Health/NPD survey revealed that only 46 percent of patients with diabetes reported having foot screenings by their primary care physician in 2012 (IPFH, 2012).
Foot Screenings and Self-Inspections
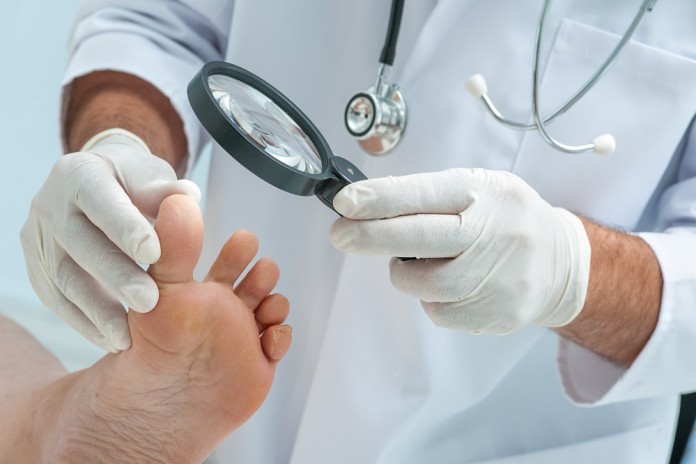
A foot screening by a primary care physician or foot health professional can go a long way toward uncovering a lesion that hasn’t healed and may be infected, or other signs, such as numbness, that could signal the need for prompt intervention. It can also reveal other issues that may interfere with the person’s quality of life or ability to be active.
Checking between the toes is critical, as doctors may uncover lesions, scaling, macerations, lacerations or existing infections. Fungal nails and skin infections also should be treated. Many doctors believe fungal nails are a cosmetic problem, but they can lead to skin infection, cellulitis and ulcers underneath the nail. Many fungal infections in the feet look similar to dry skin and calluses. Fissures in the skin can easily become infected and lead to cellulitis. Any foot infection, untreated, increases the risk of amputation, especially for those with diabetes and other conditions, such as peripheral arterial disease, which limit blood flow to the feet.
Patients also should be encouraged to do daily foot inspections themselves
Patients also should be encouraged to do daily foot inspections themselves. Experts advise those with feet at risk to do the following (American Podiatric Medical Association, Institute for Preventive Foot Health, NIH: National Institute of Diabetes and Digestive and Kidney Disease)
- Inspect feet daily. Look and feel for:
- Bumps, lumps, blisters or bruises.
- Cuts, sores, or cracked skin. Even the tiniest crack can become infected.
- Patches of thin or shiny skin (which can signal lack of blood flow) or areas of redness (especially red streaks, which can signal the presence of infection).
- Temperature differences (one part warm, another cold).
- Pain, tingling, numbness or no feeling at all.
- Ingrown toenails with red, puffy skin along the nail and tenderness or pain.
- Loss of hair on foot or leg, which can signal reduced blood flow.
- Wash feet daily with lukewarm water. After washing, dry feet thoroughly and keep them supple by applying lotion only to the tops and bottoms of the feet. Don’t apply lotion between the toes, since this can create a moist environment that favors fungal growth. Also dry between and under toes before putting on socks. If you see any sign of athlete’s foot/fungal infection, use a separate towel or tissue so the fungus does not spread to other areas of the body.
- If you can see, reach, and feel your feet, trim your toenails regularly. If you cannot, ask a podiatrist or other foot health professional to trim them for you.
- Do not attempt to cut toenails if you have neuropathy or other foot problems related to diabetes. See a podiatrist or a foot health professional regularly for toenail care and foot examinations. Never attempt to cut or file calluses or other protrusions on your feet.
- Never use wart removers or other harsh chemicals on the feet.
- Never walk or move around barefoot, even inside the house.
- Have new shoes properly measured and fitted. Foot size and shape may change over time. Shoes that fit properly are important to those with diabetes.
- Wear padded socks, without or with low-profile seams, made of acrylic or acrylic blends to protect feet and keep moisture away.
- Check inside shoes daily for sharp points, sharp edges, seams or other rough areas or foreign objects that may lead to cuts, wounds or abrasions.
- Walk as much as possible; doing so enhances circulation to the feet and helps with weight and blood sugar control.
- See a podiatrist or other foot health professional regularly—and immediately if you notice any signs of infection.
Conclusion:
Patients with diabetes are routinely referred to an eye doctor for retinopathy. However, many don’t know they might need to see a podiatrist or other foot health professional for complications of diabetic neuropathy. A timely foot screening in the primary care office is part of that care. Recognizing this, St. John Hospital and Medical Center in Grosse Pointe Woods, Michigan, initiated a Performance-Improvement Continuing Medical Education project to encourage internal medicine practitioners to do comprehensive foot exams for their diabetic patients (Szpunar et. al, 2014). Using American Medical Association methodology, the project included baseline reports about foot exam performance, an educational intervention and a reminder tool for use in practice. The project led to a significant increase in the percentage of patients who received an annual foot exam and improvements in the percentage who received a comprehensive foot exam.
References:
American Podiatric Medical Association. Diabetes; accessed Jan 7, 2016 http://www.apma.org/Learn/FootHealth.cfm?ItemNumber=980
American Podiatric Medical Association. Diabetic Wound Care; accessed Jan 5, 2016. http://www.apma.org/Learn/FootHealth.cfm?ItemNumber=981
Gemechu, F.W. et al. (2013). Diabetic Foot Infections. Am Fam Physician. Aug 1;88(3):177-184; accessed Jan 6, 2016. http://www.aafp.org/afp/2013/0801/p177.html
Institute for Preventive Foot Health. Daily Foot Care for People with Diabetes; accessed Jan 7, 2016 http://www.ipfh.org/foot-conditions/diabetes:-foot-concerns/daily-foot-care-for-people-with-diabetes/
Institute for Preventive Foot Health/NPD. 2012; accessed Jan 7, 2016 http://www.ipfh.org/resources/surveys/national-foot-health-assessment-2012
NIH: National Institute of Diabetes and Digestive and Kidney Disease. Diabetic Foot; accessed Jan 6, 2016 https://www.nlm.nih.gov/medlineplus/diabeticfoot.html
Singh, M. et al.(2005) Preventing Foot Ulcers in Patients with Diabetes. JAMA, 293(2):217-228.doi:10.1001/jama.293.2.217; accessed Jan 6, 2016. http://jama.jamanetwork.com/article.aspx?articleid=200119
Szpunar, S.M. et al. (2014) Improving Foot Examinations in Patients With Diabetes: A Performance Improvement Continuing Medical Education (PI-CME) Project. Diabetes Educ, Mar 13;40(3):281-289. http://www.ncbi.nlm.nih.gov/pubmed/24626315












Deeply concerned that the Cuban breakthrough therapy with rh-EGF intradermal infections to prevent amputation of Stage III-IV DFUs has been denied access to the USA. Furthermore, while the FDA has approved a Phase III trial in the USA, they confirm that the product would remain banned even if the Phase III trial results confirmed a reduction in amputations and an improvement in complete healing. Politics should never preclude healthcare to the people.