Peer Reviewed
Disclaimer: The authors of this report and InfectionControl.tips declare no conflict of interest with the following critical evaluation and research. No funds or influence were provided to the authors or InfectionControl.tips by any parties.
Abstract:
The spread of hospital acquired infections has been spurned by the overuse of antibiotics and the challenges of hospital cleaning. In this study, the effectiveness of an antimicrobial surface protector was evaluated. Following exposure to the Clean2Touch surface protector, it was shown that the protector was effective in reducing the growth of Staphylococcus aureus, Clostridium difficile, Escherichia coli, and methicillin-resistant S. aureus. After 2 h of incubation on the surface, there was a significant reduction in the number of viable microorganisms. Interestingly, the experiments demonstrated that a large majority of bacteria were killed instantaneously upon exposure to the antimicrobial film.
Introduction:
The World Health Organization has published numerous documents on the rising threat of antimicrobial resistance and its impact on the future global health [5]. Much of this resistance is driven by the widespread and irresponsible use of antibiotics to treat patients when they do not have a bacterial infection. The overuse of antibiotics resulted in the development and subsequent spread of drug-resistant, and more dangerously, multi-drug resistant bacteria [4, 7]. These new strains of pathogens often cause hospital-acquired infections (HAIs), which is an infection that occurs following a hospital visit [3]. In immunocompromised patients, this presents a serious and sometimes lethal threat.
Hospitals use a variety of detergents and cleansers to clean rooms in between patients. However, it requires vigilant employees to ensure that the standard operating procedures are followed and regular maintenance to remain effective in minimizing the bacterial population (bioburden) [3,9]. Due to economic reasons, employee vigilance is least emphasized by hospital administrators because it is a costly task [9]. One alternative is to maintain a low bioburden on surfaces through the application of antimicrobial surface coatings. Some systems use mechanical methods to maintain low bacterial populations. Mechanical methods reduce the bioburden without propagating antibiotic resistance or chemical tolerance as opposed to chemical or antibiotic-based solutions. In this study, we evaluate the effectiveness of a mechanical antimicrobial surface protector, Clean2Touch, in the reduction of bacteria on surfaces.
Methods:
All experiments were performed by a third party laboratory.
To evaluate the microbial load following exposure to “Clean2Touch” system, 0.4 mL of each microbial sample (Clostridium difficile, methicillin-resistant Staphylococcus aureus, Escherichia coli, and Staphylococcus aureus) at a concentration of 2.5 ×105 colony forming units per millilitre (CFU/mL) were inoculated onto sample slides with or without the treated protector. A sterile piece of plastic was placed over each inoculum to ensure even distribution of the culture. All samples, except C. difficile, were incubated at 35˚C for 24h. C. difficile was incubated at 40˚C for 24 h. Controls at time zero (prior to incubation) were evaluated for the presence of microorganisms in addition to the 24 h samples.
The number of microorganisms was tested initially by removing a 50 × 50 mm square of the sample and placing it in 10 ml tryptone soy broth. This solution was then agitated to liberate the bacteria. One millilitre of broth was inoculated onto TSA blood agar and cultured at 35˚C (40˚C for C. difficile) for 48 h. The number of CFU was evaluated at this stage.
To determine the bacteriocidal activity of the culture during short term incubation, a similar procedure was followed. E. coli and S. aureus cultures (1.9 × 106 CFU/mL and 1.9 × 106 CFU/mL, respectively) were inoculated onto a petri dish containing a 20 × 20 mm sterile sample with or without Clean2Touch film. A second, untreated piece of sterile film was placed on top of the liquid to reduce evaporation and to ensure a uniform spread of the bacterial culture. Samples were incubated for 2, 4, or 6 h. Following incubation, the upper film was removed, and the bacteria were irrigated from the sample using 10 mL of phosphate buffered saline. The number of colonies in each sample was determined from this suspension.
Results:
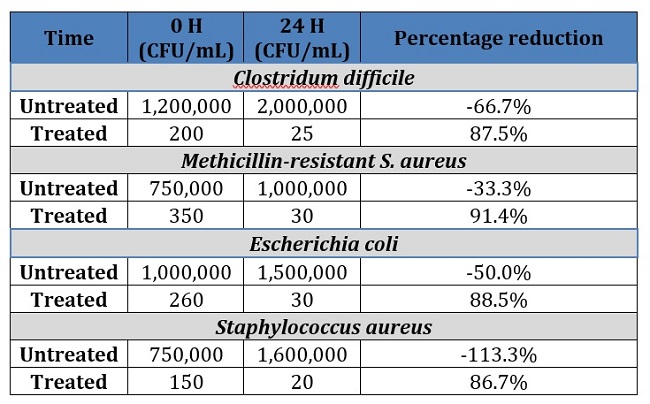
Growth of bacterial cultures on the antimicrobial film was found to be extremely limited compared to the control samples without film after a 24 h exposure period (Table 1). In samples without the film, it should be noted that all microorganisms increased in quantity, despite the lack of a growth substrate on the testing surface. Growth increased from a modest 33.3% (MRSA), up to an increase of 113.3% (S. aureus). There was a reduction in the number of bacteria on the samples containing Clean2Touch film. Reduction of the original inoculum ranged from 86.7% (S. aureus) to 91.4% (MRSA).
One interesting observation was the immediate reduction in bioburden upon inoculation onto the Clean2Touch film (Table 1, 0 H). Although there was an immediate decrease in the number of viable microorganisms following inoculation of the bacteria onto untreated samples, the decrease was highly significant when the bacteria were inoculated onto the treated surface. The original concentration decreased from 2.5 × 105 CFU/mL to an average of 2.4 × 102 CFU/mL on the treated sample, but actually increased from the same original concentration to an average concentration of 9.3 × 105 CFU/mL on the untreated samples.
Table 1. Number of viable microorganisms following culture on treated and untreated surfaces
A similar experiment was performed evaluating a shorter, more realistic exposure period. Only E. coli and S. aureus were evaluated. However, the results can be extrapolated to other microorganisms based on previous experiments. In this set of experiments, after a 2 h exposure time, the majority of E. coli and S. aureus were killed by the antimicrobial film. After 2 h, the bioburden of E. coli was reduced by 3.4 log (Figure 1). After 6 h, this was only increased to a 4.0-fold log reduction from the original inoculum. A similar trend was observed for S. aureus. After 2 h, there was a 3.3-fold log reduction in the number of viable S. aureus. However, there was >6.1-fold log reduction just after 4 hours (Figure 2). The reduction in S. aureus on the surface without antimicrobial film only exhibited a modest 0.6-fold log reduction after 2 h and a 1.1-fold log reduction after 6 h (Figure 2).
Figure 1:
Antibacterial activity of Clean2Touch Surface Protector Against E. coli
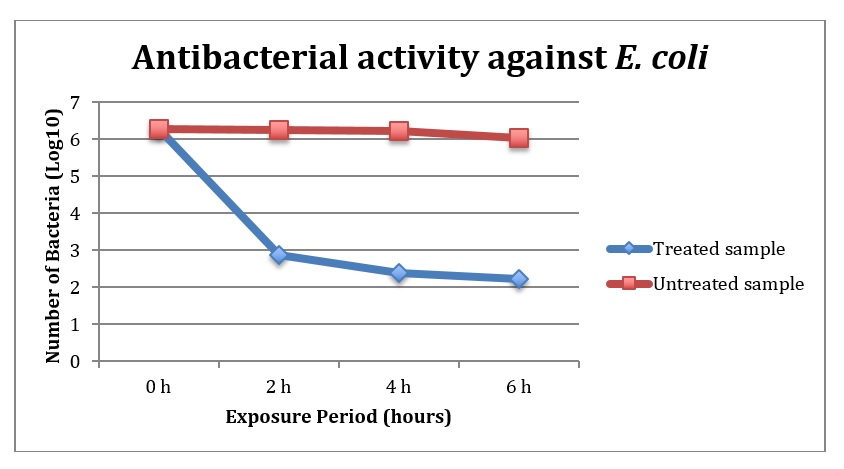
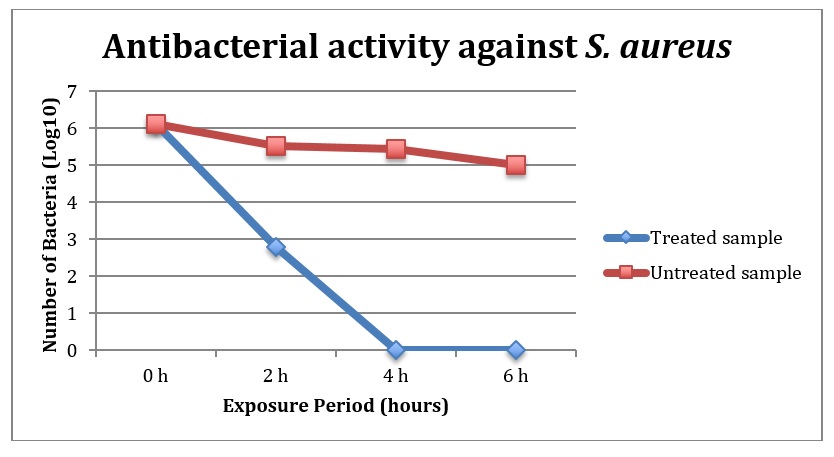
Figure 2:
Antibacterial activity of Clean2Touch Surface Protector Against S. aureus
Discussion:
The Clean2Touch antimicrobial film reduced the number of bacteria following exposure. After 24 h of incubation of bacteria on the film, there was a marked decrease in bioburden, especially for methicillin-resistant S. aureus. The same trend was observed when monitoring the number of viable bacteria with shorter exposure time. A 3-fold log (1000×) reduction in S. aureus species was observed after 2 h exposure time and this was increased to >6.1-fold log reduction after 6 h exposure.
HAIs target most patients, but especially the young, elderly, and immune-compromised patients. Although most pathogens are capable of causing HAI’s, certain species have been implicated in outbreaks [3]. The initial experiments evaluated S. aureus, E. coli, C. difficile, and methicillin-resistant S. aureus because these pathogens are considered a significant source of HAIs [2, 6]. The Clean2Touch antimicrobial film was found to be effective at eliminating all four species. It was especially effective at reducing MRSA after 24 h and S. aureus after 4 h. Only S. aureus viability was monitored at shorter time periods following exposure to the antimicrobial film. This was largely in part due to the availability of S. aureus for testing compared to MRSA. There are minimal differences between these two strains, as antibiotic resistance is conferred by small changes in the bacterial cell wall. [1,8]
The almost immediate reduction in the number of viable bacteria following inoculation on the antimicrobial film provided evidence that the film has bactericidal properties (Figures 1 and 2). There was an immediate average 3.95-fold log reduction in the number of viable bacteria. These values are very similar to the bioburden reduction observed after 2 h, which suggests that an extremely limited exposure time to the antimicrobial film may be effective for the reduction of pathogens to a safe level.
Conclusion:
The Clean2Touch antimicrobial film greatly reduced the number of viable microorganisms exposed to the film. The use of non-chemical methods to eliminate the presence of pathogens on surfaces provides hospitals and other public spaces with an innovative method for combating diseases without fueling the antimicrobial-resistance arms race.
References:
1. Chambers HF. Methicillin-resistant Staphylococcus aureus. Mechanisms of resistance and implications for treatment. Postgraduate medicine. 2001 Feb;109(2 Suppl):43-50.
2. Dancer SJ. The role of environmental cleaning in the control of hospital-acquired infection. Journal of hospital Infection. 2009 Dec 31;73(4):378-85.
3. Dancer SJ. Controlling hospital-acquired infection: focus on the role of the environment and new technologies for decontamination. Clinical microbiology reviews. 2014 Oct 1;27(4):665-90.
4. Davies SC, Fowler T, Watson J, Livermore DM, Walker D. Annual Report of the Chief Medical Officer: infection and the rise of antimicrobial resistance. The Lancet. 2013 May 11;381(9878):1606-9.
5. Knobler SL, Lemon SM, Najafi M, Burroughs T. WHO Global Strategy for Containment of Antimicrobial Resistance: Executive Summary. 2014.
6. Lobdell KW, Stamou S, Sanchez JA. Hospital-acquired infections. Surgical Clinics of North America. 2012 Feb 29;92(1):65-77.
7. Smith R, Coast J. The true cost of antimicrobial resistance. British Medical Journal. 2013 Mar 11;346.
8. Tenover FC. Mechanisms of antimicrobial resistance in bacteria. The American journal of medicine. 2006 Jun 30;119(6):S3-10.
9. Wallace N. Comprehensive Healthcare Staff Culture Survey. InfectionControl.tips. 2016 July. Accessed Aug 4, 2016 https://infectioncontrol.tips/2016/07/05/comprehensive-healthcare-staff-culture-survey/
Last Updated: October 13, 2016












