Abstract
Reduction of hospital-acquired infections is a major priority for hospital systems around the world. However, adoption of new technologies is often stunted due to acceptance of sub-optimal practices as ‘good enough.’ With lessons from past innovators, we have seen that unnecessary lives are lost when we are slow to change. This article introduces a new system for packaging and donning gloves to reduce the transfer of harmful pathogens to patients.
Introduction
Everyone in the medical or dental profession who is involved in direct patient care knows the meaning of Personal Protective Equipment (PPE). This includes protective clothing, helmets, gloves, face shields, goggles, facemasks and respirators or other equipment designed to protect the wearer from injury or the spread of infection or illness. When used properly, PPE has the potential to act as a barrier between infectious materials (like viral and bacterial contaminants) and mucous membranes, including skin, mouth, nose or eyes (US FDA, 2016).
a critical time for humankind
This comes at a critical time for humankind. With increasing numbers of mutating “superbugs” and a diminishing supply of effective antibiotics, PPE is part of a necessary expansion of patient care. Dr. Margaret Chan, Director of the World Health Organization (WHO) has stated that superbugs will have a financial/economic toll of $100 trillion dollars and a human cost of 10 million deaths (per year) in 2050 (O’Neil, 2016). This is the equivalent of a new infection every three seconds. This outpaces the mortality rate of cancer, HIV, or any other disease out there (O’Neil, 2016).
Pioneers in Early Hand Hygiene and Invention of Examination Gloves
History shows that the progress of better healthcare through the years often carries with it a struggle to bring forth a worthwhile medical process or medical device. An example of a serious struggle is Dr. Ignaz Semmelweis (July 1, 1818 – August 13, 1865). He was a Hungarian physician known today as the “savior of mothers” who discovered in 1847 that the incidence of puerperal fever, also known as childbed fever, could be drastically cut by use of handwashing standards in obstetrical clinics, saving the lives of many young mothers (Hanninen et al, 1983). While employed as an assistant to the professor of the maternity clinic at the Vienna General Hospital in Austria in 1847, Semmelweis introduced hand washing with chlorinated lime solution for interns who had performed autopsies. This immediately reduced the incidence of fatal puerperal fever from 10% range to almost two percent (Hanninen et al, 1983). At the time, diseases were attributed to many different unrelated causes. Each case was considered unique. Semmelweis’ hypothesis that a lack of cleanliness caused these illnesses was controversial at the time and was largely ignored, rejected and ridiculed (Best and Neuhauser, 2004). He was dismissed from the hospital and harassed by the medical community in Vienna, which eventually forced him to move to Budapest (Hanninen et al, 1983). Semmelweis was outraged by the indifference of the medical profession and began writing open and increasingly angry letters to prominent European obstetricians, at times denouncing them as irresponsible murderers. Semmelweis’ practices only earned widespread acceptance after his death when Louis Pasteur developed the germ theory of disease, which offered a theoretical explanation for Semmelweis’ findings (Best and Neuhauser, 2004). Semmelweis is considered a pioneer of antiseptic procedures. Since that time, resistance to the adoption of any new medical product or procedure is referred to as the Semmelweis Reflex, and is as true today as it was back then.
Dr. William Stewart Halstead, was the first surgeon in chief and one of four founding physicians of Johns Hopkins Hospital. Halstead was known for precision and cleanliness, which is why it is no surprise history credits him with developing the first surgical glove (Cameron, 1997; Osborne 2007). After his nurse, and later wife, Caroline Hampton said the chemicals she handled for surgery gave her a rash, Halstead reached out to the Goodyear Tire and Rubber Co. to create rubber gloves for her hands. Hampton loved the gloves, and more pairs arrived. Not long after, Halstead’s entire surgical staff wore them during operations. At the time, they assumed the primary benefit was increased dexterity and gave little thought to hygiene (Osborne, 2007).
Joseph Lister, the first surgeon to sterilize his surgical tools and dressings, was responsible for making surgical gloves sterile. In 1894, about 50 percent of all surgical patients died (Newsom 2003). Many of these fatalities were due to the fact that surgeons did not wash their hands between surgeries and examinations, thereby passing pathogens between patients. With the advent of sterilization of personal protective equipment, Joseph Lister had saved the lives of countless patients (Newsom, 2003).
Medical Examination Gloves and Materials
The basic types of gloves in use today include sterile and non-sterile examination and surgical gloves. The most popular types of glove materials used are nitrile, latex and vinyl. There are differences in glove packaging, usually according to the purpose of the gloves. For example, sterile gloves for general use are packaged in special wrappers that are unfolded at the point of use. These gloves are carefully removed and donned by holding on to the folded cuff of the gloves. Non-sterile examination gloves are typically packaged in boxes. These gloves are easily accessed by pulling them from opened boxes that remain open to the environment.
developing concern for health care professionals is contamination of ‘PPE’ itself
A developing concern for health care professionals is contamination of PPE itself. Gloves provide protection to both patients and healthcare workers, but unless they are certified as sterile, can become reservoirs for pathogens (Nguyen, 2016). Findings revealed that skin commensals and different types of pathogens were found left on the unused gloves (Hall et al 2014; Hughes et al, 2013).
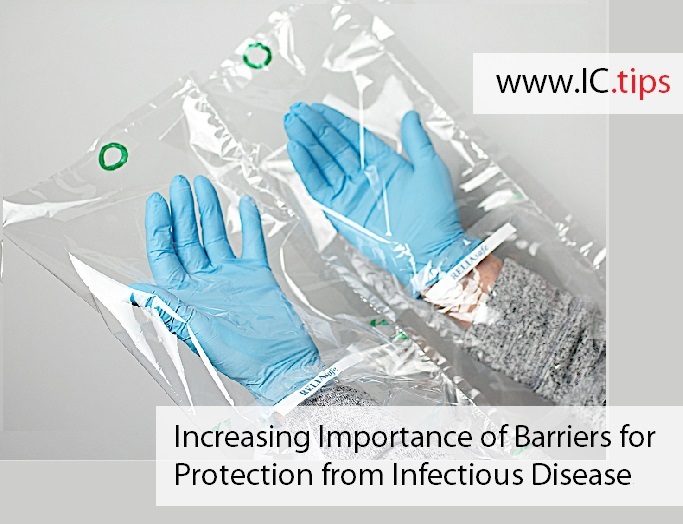
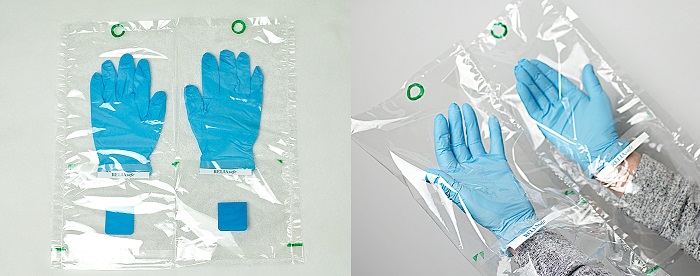
One new innovation towards reducing the spread of consists of specially designed barrier packaging that contains medical examination gloves. It is constructed from carefully selected material and features transparent internal panels that enable donning exam gloves at the patient’s bedside without contaminating the outside of the gloves (Figure 1, Liferose Products Inc). This reduces the likelihood of introducing pathogens to broken skin, mucous membranes and other entry points in patients. New innovations like this add a new dimension to PPE. It has been suggested that these products be designated PPPE or Patient and Provider Protective Equipment. This changes the current focus on safety of provider to a dual focus on patient and provider safety.
Figure 1: RELIAsafe Gloves prior to and post donning.
Conclusion and Significance
Compliance to standard care protocols exist in a perfect world, but are not always feasible in practice. Hospital acquired infections (HAI’s) are inevitable for most hospital systems, and thus preventative measures should be in place to reduce their incidence. “On average, healthcare providers clean their hands less than half of the times that they should. On any given day, about one in 25 hospital patients has at least one healthcare-associated infection” (Center for Disease Control, 2012). Shifting the priorities towards protecting workers and patients is one method of reducing the incidence of HAI’s.
The new paradigm of patient and provider protective equipment can greatly improve the outlook for patients at high risk of HAI’s. New medical barrier advances, such as the Relisafe has the potential to break the chains of infection in patient care. The unique packaging provides a convenient means of donning the enclosed gloves, immediately before initiating any medical procedures necessary for the care of healthcare patients that requires direct contact with the patient.
References
- Best, M., & Neuhauser, D. (2004). Ignaz Semmelweis and the birth of infection control. Quality and Safety in Health Care, 13(3), 233-234.
- Center for Disease Control and Prevention (2012) CDC 24/7: Saving Lives, Protecting People. Center for Disease Control and Prevention. June 6, 2012. Accessed Feb 20, 2017 https://www.cdc.gov/cdctv/emergencypreparednessandresponse/cdc-24-7.html
- Hanninen, O, Farago, M, Monos, E. (1983) Ignaz Philipp Semmelweis, the prophet of bacteriology”, Infection Control, 4 (5): 367–370
- Nguyen, U (2016) Evaluation of a Novel Non-Sterile Glove Dispensing System. InfectionControl.tips. 2, 1-8. https://infectioncontrol.tips/2016/02/24/1604/
- O’Neill J. –(May 2016) Tackling Drug-Resistant Infections Globally. Review on Antimicrobial Resistance. Accessed Feb 9, 2016. https://amr-review.org/sites/default/files/160518_Final%20paper_with%20cover.pdf
- United States Food and Drug Administration (2016) Personal Protective Equipment for Infection Control. USFDA. Accessed February 9, 2017. http://www.fda.gov/medicaldevices/productsandmedicalprocedures/generalhospitaldevicesandsupplies/personalprotectiveequipment/default.htm